I.
Temporal Bone Infections:
A.
Acute Otitis Media
Several infectious processes can affect the temporal bone and can be described on imaging by the involvement of different regions of the temporal bone: external ear,
middle ear,
internal ear/mastoid process and petrous apex.
Most common inflammatory condition of the temporal bone is acute otitis media.
Acute otitis media (AOM) is a common infection among children,
commonly caused by Streptococcus and Haemophilus Influenza,
often occurring as a disruption of the mucosal barrier due to a previous viral upper respiratory infection.
Patients usually present with fever,
otalgia and retro-auricular swelling,
as well as otorrhea.
There are no specific imaging findings,
however it may show fluid opacification of the middle ear [6] ,
tympanic membrane thickening and a bulging tympanic membrane.
Imaging studies are not recommended,
unless a complication of AOM is suspected.
In these cases,
a high-resolution computed tomography (temporal bone protocol) is performed,
which provides anatomic detail of the middle ear.
B.
Acute Otitis Externa
Acute otitis externa is most commonly caused by Pseudomonas and frequently occurs on warm and humid environments.
It has been associated to swimming in fresh-water or self-inflicted trauma.
Patients clinically present with pain,
itching and otorrhea.
Imaging is rarely required but is considered in immunocompromised or diabetic patients in order to assess for possible complications,
mainly necrotizing otitis externa.
When performed,
CT will show opacification of the external auditory canal due to edema and/or inflammation with mucosal thickening.
C.
Necrotizing Otitis Externa
Necrotizing otitis externa (NOE),
or malignant otitis externa,
is an uncommon aggressive infection,
most commonly caused by Pseudomonas.
It usually begins at the external auditory canal and extends into the soft tissues,
middle ear and adjacent bone.
It is commonly seen in patients who are diabetic,
immunocompromised or elderly.
Clinically,
patients present with fever,
otorrhea and severe unilateral otalgia.
NOE can lead to several complications including osteomyelitis,
cranial nerve palsies,
meningeal disease and dural venous sinus thrombosis.
Imaging is recommended in order to assess for extension and possible complications of the condition.
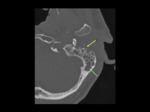
Findings include swollen soft tissues of the external auditory canal with osseous erosion and adjacent cellulitis or abscess formation.
On CT,
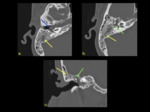
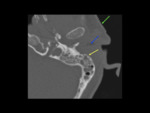
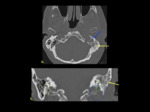
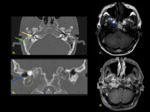
the most common finding in patients with NOE is infiltration of the medial condylar fat pad space [3].
Imaging findings also include auricle and external auditory canal (EAC) soft tissue inflammation and possible EAC bone erosion [5].
D.
Chronic Otomastoiditis
Chronic otomastoiditis is the result of persistent or recurrent episodes of acute otitis media infections leading to formation of inflammatory tissue in the middle ear and mastoid process.
Patients present with conductive hearing loss,
otorrhea or tympanic membrane perforation.
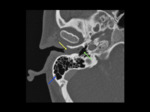
Imaging findings on CT include tympanic membrane thickening,
as well as thickening and sclerosis of the mastoid trabeculae and possible ossicle chain erosions [5].
Mastoid air cells show sclerosis or opacification.
Additionally,
middle ear changes are also seen including middle ear atelectasis or granulation tissue,
tympanic cavity erosions,
tympanosclerosis and possible development of a cholesteatoma or a cholesterol granuloma.
Chronic otomastoiditis needs to be managed adequately in order to prevent complications,
including tympanosclerosis and ossicular fixation.
II.
Complications:
A.
Coalescent Mastoiditis
Coalescent mastoiditis can occur as a complication of acute otitis media.
It is the result of the loss of the septae dividing the mastoid air cells caused by the process of demineralization and osteoclastic activity.
Subsequently,
the coalescence of the mastoid air cells can result in the formation of an empyema [3].
B.
Abscess Formation
1.
Bezold Abscess
Occurs as a complication of acute otitis media,
in which the infection erodes the cortex between the sternocleidomastoid and the posterior belly of the digastric muscles [5].
On CT,
imaging findings include a peripherally enhancing collection along with a mastoid tip defect that may lead to spread of the infection between the sternocleidomastoid and digastric muscles [5].
Early treatment should be prompted to prevent spread of the infection.
2.
Subperiosteal Abscess
Can occur as the infection extends through the cortex of the mastoid sinus.
Two locations are commonly described for subperiosteal abscess due to acute otitis media: the inferomedial location resulting in a Bezold abscess and the postauricular location occurring at the MacEwen triangle.
On CT images,
it presents as a peripherally enhancing periauricular fluid collection [3].
3.
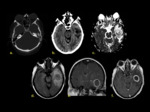
Brain Abscess
A possible complication of acute otitis media can be a brain abscess located at the temporal lobe or cerebellum.
On CT images,
it presents as a peripherally enhancing lesion.
On contrast-enhanced MRI,
brain abscesses appear as a ring-enhancing lesion demonstrating characteristic central restricted diffusion [3].
C.
Dural Venous Sinus Thrombosis
Dural venous sinus thrombosis can occur as a coexisting disease with deep venous thrombosis or cortical venous thrombosis or as a complication of acute otitis media,
among other causes.
Dural sinus thrombosis can occur due to the erosion of the sigmoid plate,
thrombophlebitis spread via emissary veins or as a complication of coalescent mastoiditis in which a secondary thrombosis can occur affecting the sigmoid sinus or internal jugular vein [3,7].
Patients present clinically with headache,
otalgia,
papilledema and fever.
Diagnosis can be made using a contrast-enhanced CTV or MRV,
in which a filling defect will be identified within the affected venous structure.
It serves to assess the extent of the thrombus.
On non-enhanced CT,
it can present with a dense triangle sign (strongly hyperdense triangle in the area of the dural venous sinus) or with a cord sign (linear hyperdense areas corresponding to thrombosed cortical veins).
On MRI,
the acute clot appears as isointense on T1-weighted sequences and hyperintense on T2-weighted sequences,
followed by the subacute clot showing T1 hyperintensity [6].
D.
Facial Nerve Involvement
Facial nerve involvement due to acute otitis media is a rare complication,
seen in less than 5% of cases and is usually completely reversible [3].
On MR,
T1-weighted images show a linear non-tumoral enhancement along the facial nerve [4].
E.
Labyrinthitis
Labyrinthitis refers to inflammation of the membranous labyrinth and can occur as a sequelae of acute otitis media due to the spread of the infection from the middle ear to the inner ear.
Labyrinthitis demonstrates three radiologic stages: [7].
- Acute stage: shows abnormal enhancement of the labyrinth on contrast-enhanced T1-weighted sequences.
- Fibrous stage: shows cochlear obstruction on CT images.
- Labyrinthitis ossificans: refers to a pathological ossification of the bony labyrinth and cochlea.
F.
Petrous Apicitis
Acute otitis media infection can spread from the middle ear and mastoid into the pneumatized petrous apex resulting in petrous apicitis.
Gradenigo Syndrome is the classic presentation of petrous apicitis with deep facial pain (due to the involvement of the trigeminal nerve at Meckel’s cave) and abducens nerve palsy (due to the involvement of Dorello’s canal) [8].
On MRI imaging,
it appears hypointense on T1-weighted sequences,
hyperintense on T2-weighted sequences and shows ill-defined enhancement on post contrast T1-weighted images [4].
G.
Cholesteatoma
Cholesteatoma can occur as a congenital lesion (2%),
or as an acquired lesion (98%) due to acute or chronic otitis media.
A cholesteatoma refers to a sac lined with ectopic stratified squamous epithelium and filled with keratin debris [7].
Acquired cholesteatomas occur more frequently on the pars flaccida of the tympanic membrane,
and can disrupt or erode the middle ear ossicles,
mastoid and scutum.
Cholesteatomas present a challenge on CT imaging since findings may be difficult to differentiate from the fluid attenuation of acute or chronic otitis media and from granulation tissue.
Diffusion weighted images help differentiate cholesteatoma and otitis media and granulation tissue.