Abstract
Cerebral vasculitis is increasingly recognized as a common cause of pediatric arterial stroke. It can present with focal neurological deficits, psychiatric manifestations, seizures, and encephalopathy. The etiopathogenesis of childhood cerebral vasculitis (CCV) is multifactorial, making an inclusive classification challenging. In this review, we describe the common and uncommon CCV with a comprehensive discussion of etiopathogenesis, the role of various imaging modalities, and advanced techniques in diagnosing CCV. We also highlight the implications of relevant clinical, laboratory, and genetic findings to reach the final diagnosis. Based on the clinicoradiological findings, a stepwise diagnostic approach is proposed to facilitate CCV diagnosis and rule out potential mimics. Identification of key clinical manifestations, pertinent blood and cerebrospinal fluid results, and evaluation of central nervous system vessels for common and disease-specific findings will be emphasized. We discuss the role of magnetic resonance imaging, MR angiography, and vessel wall imaging as the imaging investigation of choice, and reservation of catheter angiography as a problem-solving tool. We emphasize the utility of brain and leptomeningeal biopsy for diagnosis and exclusion of imitators and masqueraders.
Similar content being viewed by others
-
1.
Elucidate working classification and comprehensive discussion of the frequent and less common causes of CCV with a brief mention of their etiopathogenesis.
-
2.
Describe the precise role of various imaging modalities and advanced techniques in evaluating CCV, demonstrating the specific and nonspecific imaging findings.
-
3.
Review the genetic mutations associated with CCV and non-inflammatory vasculopathies that can masquerade vasculitis on imaging.
Introduction
Childhood cerebral vasculitis (CCV) is a heterogeneous group of vascular disorders resulting from multifactorial etiology with shared pathogenesis, i.e., vessel wall inflammation [1]. It is increasingly recognized in children with newly acquired neurological and/or psychiatric symptoms [2]. CCV has emerged as a common cause of pediatric stroke, frequently idiopathic, and may be classified in multiple ways although challenged by poorly understood pathophysiology and vague diagnostic criteria [3]. Recent research advancements evaluating inflammatory markers, cerebrospinal fluid (CSF) analysis, dedicated neuroimaging, and brain biopsy have addressed some of these issues and helped to better understand disease mechanisms. Vessel wall imaging (VWI) is a promising tool to assess medium to large vessel disease, but biopsy is usually needed for small vessel vasculitis [4]. In this article, we describe the salient imaging findings that help narrow the differential diagnostic possibilities and facilitate CCV diagnosis. We also recommend a stepwise clinicoradiological evaluation and a working classification based on literature review and personal experience to guide appropriate management.
Classification
The classification systems for CCV are diverse and the subject of an ongoing debate. Central nervous system (CNS) vasculitis has traditionally been classified as primary CNS vasculitis, idiopathic with isolated CNS involvement and secondary CNS vasculitis as a part of systemic disease due to numerous entities, including rheumatological, infective, drug or treatment-related causes [5]. Currently, CCV is classified based on [1] etiology, into primary/idiopathic and secondary; [2] histological pattern, into granulomatous and non-granulomatous [3]; vessel size, into small, medium, or large vessel vasculitis [4]; clinical phenotypes, into primary and secondary vasculitis as well as [5] disease course, comprising transient, non-progressive or progressive, and monophasic or recurrent types [6].
Diagnostic Assessment
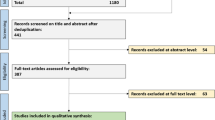
CCV is rarely a prospective diagnosis and is mostly presumed after initial evaluation. The confirmed diagnosis would require detailed laboratory evaluation (blood work and CSF), imaging studies, and in most cases, histopathological evaluation to confirm the diagnosis [7]. A step-by-step diagnostic algorithm (Fig. 1) for evaluating suspected CCV is desirable, incorporating laboratory and imaging findings. Brain and leptomeningeal biopsy remains the reference standard and is performed in suspected cases with inconclusive clinicoradiological assessment [8].
Diagnostic algorithm for the evaluation of suspected Childhood Cerebral Vasculitis. CSF cerebrospinal fluid, vWF von Willebrand factor, MRI magnetic resonance imaging, MRA magnetic resonance angiography, VWI vessel wall imaging, CNS central nervous system, cPACNS childhood primary angiitis of the central nervous system
Laboratory Evaluation
Laboratory analysis, especially the cell counts and inflammatory markers in the blood and the CSF, coagulation profile, and liver and renal function tests are non-diagnostic due to lack of specificity and support the presumptive diagnosis of CCV [1, 9]. The main role is to rule out pre-existing diseases, systemic vasculitis, infections, or drug toxicity. It also helps predict the disease activity, treatment response, and prognosis [7].
Blood Investigations
Frequently utilized blood tests include complete hemogram, inflammatory biomarkers (leukocyte counts, CRP, ESR), bleeding and coagulation profile, liver and renal function tests. The toxic-metabolic screen and antibody titer assessment (anti-nuclear antibody [ANA], anti-neutrophilic cytoplasmic autoantibodies [ANCA], anti-phospholipid antibody [APLA]) should be performed to rule out secondary vasculitis [10]. The inflammatory biomarkers are more frequently abnormal in secondary CCV and angio-negative childhood PACNS (AN-cPACNS) than angio-positive childhood PACNS (AP-cPACNS), suggesting relatively limited inflammation in AP-cPACNS [11]. Von Willebrand factor (vWF) is a well-established marker in cPACNS, mirroring disease activity and helps assess the treatment response and prognosis [12].
CSF Analysis
CSF parameters reflect the CNS biochemical milieu and reveal ongoing disease processes. They can suggest a specific diagnosis and rule out etiologies such as infections, inflammatory brain diseases, and neuronal or autoantibody-related disorders, including systemic vasculitis, rheumatoid disease, demyelination, and autoimmune encephalitis [9]. The CSF inflammatory biomarkers (leukopleocytosis, normal/decreased sugar, elevated protein, oligoclonal bands) are more frequently abnormal in secondary CCV and AN-cPACNS compared to AP-cPACNS [10,11,12,13].
Imaging Evaluation
Imaging modalities, including ultrasound Doppler, CT, MRI, and catheter angiography (CA) play a quintessential role in the detection and classification of CCV.
Ultrasound Doppler
Helps assess extracranial medium to large vessel wall thickening, flow abnormality, and luminal stenosis [14].
CT
Non-enhanced CT has a limited role. In an emergency setting, it rules out hemorrhage or infarction [15]. Contrast-enhanced CT and CTA may demonstrate enhancing parenchymal lesions, leptomeningeal enhancement, and vascular abnormality; however, CECT/CTA is not usually preferred in children due to limited vessel wall assessment and radiation exposure [14, 16, 17].
MRI
Investigation of choice to assess suspected CCV. It can demonstrate parenchymal changes (edema, infarction, and microhemorrhages), vascular abnormalities by evaluating involved vessel size, wall enhancement pattern, and outlining ancillary findings, including leptomeningeal enhancement [5, 18,19,20]. The cross-sectional (CT and MR) angiographic techniques are not reliable in the evaluation of the distal intracranial arteries. It is challenging to differentiate CCV from other causes of luminal narrowing, including reversible cerebral vasoconstriction syndrome (RCVS), especially in the absence of vessel wall imaging (VWI) which further reduces the accuracy [21,22,23,24]. The inclusion of VWI increased the diagnostic accuracy of MR angiography (MRA) from mere 8.3% to 95.8% in identifying vasculitis [25].
VWI is crucial for precisely assessing vessel wall thickening and enhancement and helps differentiate inflammatory vasculitis from other mimics, including non-inflammatory vasculopathy [14, 15]. The technical considerations for VWI vary depending on the magnetic field strength and various hardware configurations. The important considerations to achieve the higher spatial resolution and signal to noise ratio include a 3T or higher magnetic field strength, a 32 or 64-channel head coil over an 8 or 12-channel head coil to increase peripheral resolution, along with combination of a precontrast and postcontrast T1-weighted anisotropic 2D and isotropic 3D sequences based on the specific clinical indication [26, 27]. An important consideration in performing VWI, specifically in younger patients, in the evaluation and follow-up of CCV includes repetitive use of gadolinium-based contrast agent [28]. The role of dedicated MR sequences in the evaluation of CCV is summarized in Table 1.
Catheter Angiography (CA):
Excellent for diagnosing and assessing most vascular disorders [15, 20]; however, its use is limited in children due to the invasive nature and technical difficulties. Moreover, small-vessel vasculitis may not be apparent on CA with the sensitivity and specificity in detecting PACNS being as low as 27% and 30%, respectively [1, 20, 29, 30].
Histopathological Evaluation:
Meningocortical biopsy is the reference standard to confirm the diagnosis and rule out other etiologies, and mimics [1, 14, 20]. Due to the absence of affirmative imaging findings and laboratory tests, compounded by the nonspecific presentation, biopsy is mostly indicated in AN-cPACNS. The vessel wall demonstrates an inflammatory disease process suggesting the histological diagnosis of vasculitis. In cPACNS, vessel wall inflammation may be granulomatous, non-granulomatous, or both. Unlike adults, the non-granulomatous form is predominant with T‑cell lymphocytic infiltrates in children [5, 19, 31]. Wherever possible, biopsy is generally lesion-targeted, but due to diffuse cerebral vascular distribution of affected and unaffected areas on imaging, it can be done anywhere in the brain in AN-cPACNS [11, 31, 32]. The tissue biopsy, however, has low sensitivity with a higher false negative rate of up to 25% due to diffuse patchy involvement of the cerebral parenchyma [30].
Imaging in Childhood Cerebral Vasculitis
In this article, we classify CCV into two broad categories, primary and secondary CNS vasculitis. The primary CNS vasculitis, also known as primary angiitis of CNS (PACNS), is further classified into small or large vessel disease based on the angiographic appearance with a progressive or non-progressive clinical course [1]. Based on etiopathogenesis and vessel size involvement, secondary CNS vasculitis is subclassified into four major groups [5, 11]. We also describe non-inflammatory vasculopathy with imaging appearance of vasculitis but lacking vessel wall inflammation and uncommon genetic mutations [24,25,26, 34, 35]. Lastly, we describe a few commonly encountered CCV mimics that confound the diagnosis (Table 2).
Primary CNS Vasculitis
Childhood-PACNS (cPACNS) is a rare cerebral vascular disease and is now considered one of the common causes of pediatric stroke. The exact incidence of cPACNS is not known; however, it constitutes up to 24% of stroke in children compared to 0.5% in adults [36]. It is an inflammatory disease process limited to cerebral vessels (arterial wall and perivascular spaces). Although often idiopathic, it may be infrequently associated with infectious (HIV, HCV) and non-infectious autoimmune diseases [5, 36, 37]. It was first described in 1959, affecting adults [38], and later recognized in children [39]. Multiple diagnostic criteria have been proposed, and the most recently adopted criteria include newly acquired neurological deficits or psychiatric symptoms in patients under 18 years with specific angiographic and/or histopathological features of CNS vasculitis in the absence of an underlying systemic disorder or extra-CNS involvement [2, 5, 36].
cPACNS is classified into large or angio-positive (AP-cPACNS) and small or angio-negative (AN-cPACNS) disease based on the affected vessel size [36, 40]. Depending on the disease evolution, large vessel or AP-cPACNS is subdivided into non-progressive (APNP-cPACNS) and progressive (APP-cPACNS) forms [5, 36]. Histopathologically, small vessel cPACNS (AN-cPACNS) can be subdivided based on the involvement of arterioles, capillaries, and venules [11]; however, the initial diagnosis of cPACNS subtypes is evasive due to significant overlap in the clinical, laboratory, and imaging findings. The definitive diagnosis is based on the combination of criteria and pathological analysis.
Clinical Features
cPACNS can present with diverse neurological symptoms including acute stroke-like presentation, commonly in non-progressive (APNP-cPACNS) form. Headache and seizures are more frequent in progressive (APP-cPACNS) form owing to subacute nature and multifocal involvement [1, 9, 11, 18, 40, 41]. AN-cPACNS has a gradually progressive course and often presents with seizures, encephalopathy, and neuropsychiatric abnormality due to diffuse CNS involvement [1, 4, 11, 40]. Angio-negative vasculitis is more common in girls whereas angio-positive vasculitis is frequently observed in boys, possibly explaining the male preponderance in pediatric stroke [1, 5, 11].
APNP-cPACNS is the most common subtype encountered in children [11]. It has a better prognosis than other forms of cPACNS with a limited course [11, 18]. The most common imaging findings are ischemic parenchymal lesions in the proximal anterior circulation (gangliothalamic), angio-positivity with characteristic unilateral proximal vascular involvement, and relative sparing of the distal segments [9, 11, 36, 42, 43]. VWI may demonstrate circumferential wall thickening and enhancement. Posterior circulation, posterior fossa, and spinal cord involvement are extremely uncommon; seldom, there is a meningeal and parenchymal enhancement [7].
APP-cPACNS, the protracted form of cPACNS, involves both proximal and distal arterial segments [19]. The diagnosis is usually based on imaging findings favoring vasculitis after excluding secondary causes. MRI can depict ischemic lesions in a unilateral or bilateral hemispheric distribution (Fig. 2), involving proximal or distal, anterior or posterior circulation arteries with no specific imaging pattern [11, 18, 44]. Isolated posterior fossa and spinal cord involvement are not uncommon [11, 45]. At the active inflammation sites, vessel wall, meningeal and parenchymal enhancement may be seen [21, 46]; however, parenchymal hemorrhages are infrequent in children [5, 11, 18, 19].
APP-cPACNS in a 10-year-old boy presented with recurrent stroke. Axial DWI (a) image shows multifocal right frontoparietal border-zone infarcts (arrows). MRA (b) shows diffuse narrowing of the right distal internal carotid artery (ICA), middle cerebral artery (MCA), and anterior cerebral artery (ACA) (arrows). Previous MRI, 4 years ago reveals left periventricular (arrow) white matter infarct on DWI (c) and occlusion of A1 segment of left ACA (dashed arrow in b)
AN-cPACNS is a chronic disease with a slower progressive course, more frequent cognitive dysfunction, and greater mood instability due to more widespread CNS involvement [1, 47]. The diagnosis can be challenging due to its insidious onset and vague presentation, frequent seizures, nonspecific imaging findings, multifocal demyelination-like pattern, and angio-negativity [1, 4, 11, 19, 29, 37, 40, 46, 47]. vWF reflects the disease activity and helps rule out CCV mimics like demyelinating disease [10, 12, 13]. MRI is the investigation of choice, but biopsy is often required for diagnosis. Imaging studies demonstrate multifocal infarcts in one or both cerebral hemispheres with normal appearing vessels on MRA and VWI (Fig. 3). Posterior fossa and spinal cord may be involved, presenting as cerebellitis or transverse myelitis [11, 45]. Leptomeningeal enhancement is also frequent. CA is inconclusive, and biopsy is usually needed for diagnosis. Unlike adults, non-targeted brain biopsy in children has a similar yield to the targeted lesional biopsy due to widespread brain involvement [31, 32, 48].
Management
The cPACNS shows an adequate response to anti-thrombotic and anti-inflammatory therapy, preventing luminal occlusion and vessel wall inflammation, respectively [1, 11]. Unlike the non-progressive form, the progressive cPACNS requires longer therapy and immunomodulators in refractory cases [1, 41, 49, 50]. AN-cPACNS also requires prolonged treatment (2–3 years) similar to the progressive cPACNS, with or without anti-epileptics [13, 51]. Follow-up is performed with laboratory parameters, particularly vWF; MRI is done to evaluate the residual disease and assess disease stability at 3 months for non-progressive form and every 6 months in progressive form [11, 18]. AN-cPACNS is usually monitored by clinical response and laboratory parameters. Follow-up imaging is not necessary but may be performed depending on initial imaging findings and clinical status [1, 11, 13]. An elaborative discussion of the therapeutic management of cPACNS is beyond the scope of this review [1, 11, 13, 18, 41, 49,50,51].
CCV Secondary to Infections
Infections are the most common cause of secondary CCV and may be viral, bacterial, fungal, or parasitic in origin [11, 52]. Infections may affect the vessel wall due to direct invasion (Mycobacterium tuberculosis, Varicella zoster, HIV, and Lyme disease) or by inciting an inflammatory response (bacterial and viral meningitis) releasing inflammatory markers [1, 53]. The clinical symptoms include fever, headache, seizures, stroke, and encephalopathy. Laboratory evaluation is paramount to establish the causative organism and guide appropriate management [52]. The CSF opening pressure and analysis (DNA, antigen, and antibody) can help establish organisms limited to the CNS. On VWI, the affected arteries may show segmental narrowing, occlusion, aneurysmal dilatation, and wall enhancement. In addition, there may be associated parenchymal changes and meningeal enhancement [14, 54].
Bacterial meningitis (most commonly groups A and B Streptococcus) may cause vasculitis and cerebral infarcts (Fig. 4a) in up to 30% of children [55]. Focal cerebral arteriopathy (usually unifocal) and ischemic stroke (Fig. 4b,c) are the most common features of childhood post-varicella angiopathy [56, 57]. Spinal cord (VZV myelitis) and peripheral nervous system involvement can occur but are exceptional in children. The reported incidence of Ramsay-Hunt syndrome in young children is about 2.7/100,000 [58, 59]. In children, Mycobacterium tuberculosis is one of the common causes of chronic meningitis leading to vasculitis and vasculitic infarcts due to thick enhancing basal cistern inflammatory exudates involving perforating arteries and the circle of Willis [14]. HIV-associated cerebral vasculopathy is usually associated with severe immunosuppression or vertical transmission [14]; and demonstrates vascular narrowing, aneurysms, thromboembolism, and parenchymal changes [60]. Fungi are important CNS pathogens in the background of leukopenia and immunosuppression, and the presence of co-existing sinonasal or orbital disease favors the diagnosis [14]. Less is known about CNS involvement in pediatric SARS-CoV‑2. Various patterns are described, including cerebral vascular involvement, resulting in inflammatory vasculitis and vasculitic infarcts [61]. The treatment of infectious vasculitis is usually organism-specific along with antithrombotic and anti-inflammatory therapy. Serial vascular imaging, usually MRA with or without VWI, is necessary to assess disease progression and treatment response [15].
a 11-year-old girl with group A streptococcal meningitis. TOF-MRA reveals attenuation of bilateral MCA, right (arrows) more than left. Enhancing basal exudates and leptomeningeal enhancement are also noted in postcontrast T1W image (inset image). b,c 6-year-old boy with left hemiparesis and history of varicella. Axial DWI image (b) shows acute infarction of the right posterior gangliocapsular region (arrow in b) with narrowing and irregularity of the distal most intracranial segment of the right ICA and origin of right ACA (dashed oval in c) in keeping with post-varicella focal cerebral arteriopathy
CCV Secondary to Systemic Vasculitis
CCV associated with systemic vasculitic processes are generally divided into small, medium, large, and variable sized vessel vasculitis (Table 2) based on the predominantly affected vessel size [3, 8, 14, 15, 54, 62]. The most common causes of pediatric systemic vasculitis are Henoch-Schönlein purpura, Kawasaki disease, and Polyarteritis nodosa (PAN). The clinical presentation depends on the involved vessel size and extra-CNS disease severity [20]. The large and medium vessel involvement usually present with stroke-like symptoms, neurological deficits, and encephalopathy. Small vessel vasculitis is subdivided into ANCA-positive or ANCA-negative and frequently presents with craniospinal neuropathies [15]. Laboratory analysis is essential for disease diagnosis and differentiates various subgroups based on specific antibodies (ANA, anti-double stranded DNA, dsDNA, ANCA) [63]. Imaging findings depend on the involved vessel size, disease phase, and disease-specific features. Immunomodulatory therapy is usually guided by organ-specific involvement and associated complications.
Takayasu arteritis (TA) is still the most common large vessel vasculitis in childhood and can also be seen in infancy [64]. Hypertension is the most frequent presentation due to renal arterial involvement. Craniocervical arteries are the second most commonly involved, more commonly involving extra-cranial than intracranial arteries. Intracranial arterial involvement manifests clinically as stroke-like episodes, usually in the second decade with female preponderance [65, 66]. The diagnosis is frequently radiological, demonstrating typical vascular imaging findings with arteries showing characteristic mural thickening and enhancement in the acute phase with multiple fibrostenotic and dilated segments in the delayed phase with or without collateral formation [14, 62, 67].
Kawasaki Disease (KD) is the most common medium vessel vasculitis in children younger than 5 years with highest incidence of 239 per 100,000 under 5 years in the Japanese population [3]. Up to 30% present with CNS involvement [68, 69]. KD is often diagnosed using clinical criteria and echocardiography in a febrile child. Imaging findings are nonspecific, with frequent MRI findings of meningoencephalitis. In an appropriate setting, the presence of splenial involvement and diffuse microhemorrhages favor the diagnosis of KD [70].
Childhood PAN is associated with HBV and a recently identified genetic cause, i.e., ADA2 deficiency due to autosomal recessive CECR1 gene mutation [71]. Based on multiple clinical and laboratory criteria, the American College of Rheumatology (ACR) proposed diagnostic criteria for PAN. CNS involvement is seen in the severe systemic variant of childhood PAN [72, 73]. Childhood PAN most frequently presents with focal or multifocal ischemia and hemorrhage with typical vascular findings (Fig. 5), including wall thickening, small aneurysms, and stenosis [14].
4‑year-old male with ADA2 mutation. Axial DWI image (a) reveals acute infarct of the posterior limb of left internal capsule (arrow). Axial VWI image (b) shows wall thickening and enhancement (arrows) of the intracranial vessels. Contrast MRA (c) shows a small saccular aneurysm of the left anterior choroidal artery with a filling defect from thrombus (arrow) that was not appreciated on the TOF-MRA (not shown). MRA of the abdominal vessels revealed multiple aneurysms of the gastric, renal, and splenic arteries (not shown) in keeping with PAN
Small vessel vasculitis is further subclassified based on ANCA status. Although ANCA-negative vasculitis is more frequent in childhood, CNS involvement is more frequent with the ANCA-positive subtype [74]. The diagnostic criteria are clinicoradiological and may require histopathology based on the ACR/EULAR classification. ANCA-positive vasculitis includes granulomatosis with polyangiitis, previously Wegner granulomatosis (GPA-cANCA), microscopic polyangiitis (MPA-pANCA) and eosinophilic granulomatosis with polyangiitis, previously Churg Strauss syndrome (EGPA-pANCA). CNS involvement ranges between 10 and 20% and often manifests with pachymeningitis, ischemic lesions, vascular changes (Fig. 6a,b), and cranial neuropathies [74]. Few imaging findings may point to a specific diagnosis. For instance, an enlarged pituitary gland, orbitonasal involvement, and cranial neuropathy (optic and olfactory nerves) suggest GPA [74, 75]; and an ischemic optic neuropathy is associated with EGPA [76]. CCV secondary to MPA is scarce, with only a few cases in the literature [77].
a,b 8-year-old boy, ANCA-positive glomerulonephritis with headache and seizures. Axial FLAIR image (a) shows multiple bilateral subcortical and deep white matter hyperintensities, few involving the cortex (arrows) with restricted diffusion on DWI (not shown). TOF-MRA (b) depicts mild irregularity of bilateral ACA, most prominently involving the A1 segment of right ACA (arrow). c 11-year-old boy, known Behçet disease presented with right trochlear nerve palsy and anterior uveitis. Axial FLAIR image shows mildly expansile hyperintense lesion of the midbrain, centered over left inferior colliculus (arrow) suggestive of neuroBehçet
Henoch-Schönlein purpura is an ANCA-negative small vessel disease with infrequent CNS involvement. It is usually secondary to hypertensive or uremic encephalopathy and presents with PRES-like imaging findings [78].
Pediatric onset Behçet’s disease (BD) has a strong genetic and HLA-B51 association [79]. The prevalence of Behçet’s disease is extremely variable, estimated to be about 10.3/100,000 globally, ranging from as high as 119/100,000 for Turkey to as low as 3.3–3.8/100,000 for Europe and North America [3, 80]. CNS involvement is seen in up to 30% of pediatric BD and may present with nonspecific headaches and psychiatric manifestations. It has a chronic waxing-waning course that mimics multiple sclerosis (MS) and can involve any vessel, including veins [81]. The most common imaging findings are venous sinus thrombosis and angiocentric brainstem lesions (Fig. 6c), with or without hemorrhage and enhancement [79, 81]. The diagnostic criteria for pediatric BD have recently been modified to exclude the pathergy (skin) test and include radiological findings (arterial or venous thrombosis and arterial aneurysms) [15, 79].
CCV Secondary to Systemic Inflammatory Disease
Inflammatory disorders are increasingly associated with CCV, particularly in pre-existing Systemic lupus erythematosus (SLE), Sjögren’s syndrome (SS), Systemic sclerosis (SSc), Juvenile dermatomyositis (JDM), Mixed connective tissue disorders (mCTD), Inflammatory bowel diseases (IBD) and Hemophagocytic lymphohistiocytosis (HLH). The clinical presentation is nonspecific with increased inflammatory markers and disease-specific antibodies that may point to a specific diagnosis (anti-topoisomerase and SCL-70, in SSc, anti-dsDNA in SLE, myositis-specific antibodies (MSA) in JDM, and anti-Ro and anti-La in SS). MRI with MRA is the imaging of choice and demonstrates multifocal cortical-subcortical involvement with or without vascular changes [11, 14, 15, 54]. The treatment is aimed at the primary disease process and its visceral and systemic complications.
Juvenile SLE is a common systemic inflammatory disease with a few studies demonstrating cerebral parenchymal involvement in up to 75% of patients and frequent neuropsychiatric features [14]; however, vasculitis (Fig. 7a,b) is encountered in about 10% of cases [82]. SLE with positive APLA may result in small and medium vessel thrombosis, manifesting clinically as antiphospholipid syndrome (APS) (Fig. 7c), requiring anticoagulation in up to 50% [15, 82]. The APLA titer assessment (along with anti-dsDNA) is warranted in SLE presenting with thrombo-occlusive vasculopathy [82].
14-year-old female with SLE, recent onset behavioral changes and positive APLA titer. TOF-MRA (a) demonstrates mild irregularity of intracranial arteries especially the M1 segments of the bilateral MCA (arrows) with poor visualization of peripheral arteries and normal brain parenchyma (not shown), similar to previous MRI. TOF-MRV (b) and post-gd T1W (c) images show interval development of the narrowing of right internal jugular vein (IJV), starting from the junction of IJV & sigmoid sinus (arrows) with non-visualization at the level of C1–C2 (arrow) compared to normal IJV on left side (dashed arrow) in keeping with clinical diagnosis of APLA syndrome
Juvenile SSc can have extracutaneous involvement, but CNS involvement is exceptional and may present as ischemia, infarction, or hemorrhage [14]. Diagnosis is clinical, ANA testing is sensitive but not specific, and SCL-70 antibodies are relatively specific but positive in 15–20% of patients only [83].
CNS involvement in pediatric SS is infrequent, and the CSF anti-Ro and anti-La antibodies aid in diagnosis [14, 84]. Imaging findings are nonspecific (Fig. 8), but the spinal cord and optic tract (mimicking MS) along with glandular involvement suggest the diagnosis of pediatric SS [84].
9‑year-old girl with Sjögren syndrome and anti-Ro positive, presents with vomiting and gait disturbance. Axial FLAIR images show multiple cortical-subcortical white matter hyperintensities involving bilateral cerebral (arrows in a), brainstem, and cerebellar hemispheres (arrows in b). Imaging of the spine demonstrated similar changes in the distal cord and conus (not shown)
Juvenile dermatomyositis (JDM) is the commonest idiopathic inflammatory myopathy. In JDM, CNS vasculitis is extremely rare among inflammatory diseases, presenting with seizures and psychiatric symptoms and may be life-threatening [85]. Imaging findings are nonspecific; however, retinal vascular involvement favors diagnosis of JDM. Various MSA are positive in JDM (frequently anti-NXP2 in children), showing a predilection for a particular organ or system, but none specific to CNS [86].
CNS involvement in pediatric IBD is extremely uncommon as Crohn’s disease, the predominant type of IBD in children, is rarely associated with CNS vasculitis. Also, ulcerative colitis, frequently associated with CCV, usually occurs beyond adolescence [87].
Hemophagocytic lymphohistiocytosis (HLH) is a non-cancerous, hyperinflammatory condition characterized by uncontrolled lymphocyte and macrophage proliferation with familial (genetic) and acquired forms. CNS involvement is seen in up to 73% with or without systemic involvement and may be categorized into two MRI imaging patterns [11, 88]. Pattern I (significant parenchymal disease) subdivided into multifocal white matter, brainstem-predominant, and cerebellitis group. Pattern II shows non-specific imaging findings [89]. Three histopathological stages of CNS-HLH are described with perivascular enhancement in a few stages, similar to small vessel CNS vasculitis [88]. Imaging findings are nonspecific and histological confirmation is almost always required.
CCV Secondary to Neoplasms, Drugs, and Treatment-related
This heterogeneous group of CCV is commonly caused by illegal and therapeutic drugs (including chemotherapy), radiation therapy, malignancy, and graft versus host disease (GVHD). The clinical presentation can be subtle or bizarre, mimicking an unrelated disease process. The history may be unreliable in substance abuse, and laboratory assessment could help identify the specific agent. Neuroimaging findings are nonspecific and depend on the underlying etiology.
Drug-related CCV usually affects small to medium-sized arteries and frequently presents with multifocal infarcts, and intracranial hemorrhage (cocaine and methamphetamine) (Fig. 9). Moyamoya-like vasculitic changes may be seen with chronic cocaine abuse [11, 14, 15, 54].
Radiation vasculopathy is a slowly evolving disease, seen in approximately 6.7% of post-radiotherapy cases. Usually, the medium to large-sized arteries are affected, resulting in vascular narrowing and ischemia ([14]; Fig. 10). Histopathologically, the involved arteries show foam cell collections and myointimal proliferation. VWI demonstrates wall thickening and enhancement, which improves with time and treatment [54].
Malignancy-related CCV is infrequent and usually seen with lymphoproliferative malignancies, mostly manifests as GVHD and increasingly recognized due to a surge in hematopoietic stem cell transplantation (HSCT) [11, 90]. Cerebrovascular complications include ICH, arterial stroke, venous thrombosis, and PRES-like features secondary to microvascular endothelial injury or vasculitis. These complications are frequent in the pre-graft (< 30 days) and early post-graft period (30–100 days) [90].
Rare Mutations Presenting as CCV
In children and young adults, rare genetic and sporadic mutations causing CCV are often overlooked and should also be considered [11]. Family history may help identify the cause, and genetic analysis is confirmatory. Imaging findings are variable; however, few of these mutations have characteristics vital to a specific diagnosis. Treatment is based on underlying diagnosis and their complications [11, 54].
ADA2 mutation results in adenosine deaminase‑2 deficiency due to cat’s eye syndrome chromosome region 1 (CECR1) gene mutation on chromosome 22 [71]. It presents with PAN-like systemic inflammatory syndrome (Fig. 5) with early and frequent CNS involvement resulting in multiple intracranial aneurysms and stroke [11, 33]. The autoimmune PAN-like illness from ADA2 deficiency responds well to anti-TNF therapy [91].
ACTA2 mutation occurs due to Arg179His mutations with resultant multisystem smooth muscle dysfunction [92]. It presents with salient findings of prominent proximal extradural ICA, straight and narrow intradural vessels without basal lenticulostriate collaterals (contrary to moyamoya disease) [91, 93]. The typical parenchymal changes include dysplastic anterior corpus callosum, radial frontal gyration, thickened and flattened fornix, basilar artery indentation causing pontine flattening (twin peak sign) (Fig. 11), and squeezed midbrain [92, 93].
13-year-old boy with ACTA2 mutation. Axial T1W image (a) shows V‑shaped anterior corpus callosum (dashed line) and thickened fornix (arrow). Axial T2W image (b) shows twin peaks sign from impression of the stretched basilar artery (dashed oval). TOF-MRA (c) depicts fusiform dilatation of the bilateral proximal ICAs (arrows), with tapering of terminal segments. Bilateral ACA, MCA, PCA, and their branches appear attenuated and stretched
MYH11 mutation is an extremely rare disorder leading to smooth muscle dysfunction that can affect cerebral vessels like ACTA2 mutation, with similar neuroimaging findings. Cardiovascular involvement is frequent, including thoracic aortic aneurysm and patent ductus arteriosus [91].
Aicardi Goutières syndrome is a genetic condition caused by mutations in TREX1, SAMHD1 RNASEH2A, RNASEH2B, RNASEH2C, ADAR1, and IFIH1 that presents with variable leukoencephalopathy. The SAMHD1 mutation often presents with neurological regression and vasculitis-like features with characteristic beading of MCA associated with white matter changes, calcification, and atrophy with progressive microcephaly [11, 34, 94].
Non-inflammatory Vasculopathy
Non-inflammatory vasculopathies mimic vasculitis with similar vascular and parenchymal changes; however, the absence of wall enhancement and inflammatory markers help distinguish from CCV and diagnose non-inflammatory vasculopathy, including moyamoya disease, fibromuscular dysplasia, and connective tissue disorders (CTDs) [10, 81].
Moyamoya Disease:
A vascular dysplasia resulting in progressive narrowing and stenosis of the terminal ICA and proximal segments of anterior and middle cerebral arteries, resulting in multiple fragile leptomeningeal and extensive deep collaterals (Fig. 12; [15, 91]). The leptomeningeal collaterals appear as FLAIR sulcal hyperintensity, i.e., ivy sign, with deep perforating collateral arteries manifesting as “puff-of-smoke” appearance on angiography [54]. Ischemic changes with watershed involvement are frequent in children with infrequent hemorrhagic infarction than adults [15, 16]. It can be idiopathic with ethnic and familial predisposition or secondary to various somatic and genetic conditions, including neurofibromatosis, tuberous sclerosis, Down syndrome, thalassemia, and sickle-cell disease [18, 81].
a Moyamoya syndrome in an 11-year-old boy with sickle cell disease. TOF-MRA shows marked narrowing and beaded appearance of the bilateral MCA with asymmetric narrowing of the supraclinoid ICA, right \(\gg\) left (arrows) and multiple tiny basal collaterals (dashed oval). b Idiopathic Moyamoya disease in 10-year-old boy presented with progressive right-sided weakness. TOF-MRA reveals narrowing and irregularity of the supraclinoid portion of both ICA. The origin of bilateral MCA (arrows) and ACA are not well seen (R > L) and are replaced by a network of tiny tortuous collaterals (dashed oval). Left PCA also appears attenuated (dashed arrow) with prominent and tortuous posterior communicating arteries
Fibromuscular Dysplasia (FMD):
Usually affects medium to large arteries, frequently resulting in alternating stenosis and post-stenotic dilatation and/or aneurysm, giving the classical “string of beads” appearance on CTA/MRA [15, 54]; however, this typical appearance is frequently absent in children due to isolated intimal hyperplasia, a rare pathological subtype, compared to medial and/or perimedial fibroplasia in adults [95]. Cerebral vascular disease is infrequent in children with more frequent posterior circulation involvement. FMD shows no gender predisposition in children with most commonly affected vessels in order of arterial involvement, renal, craniocervical, non-renal visceral, and limb arteries [15, 54].
Vasculopathy Associated with Connective Tissue Disorders
TGF-β Signaling Pathway
Marfan Syndrome:
Autosomal dominant (AD) inherited CTD resulting from fibrillin‑1 gene mutation on chromosome-5 affecting the TGF‑β pathway [15, 35, 54]. It frequently presents with craniocervical ectasia and aneurysms (Fig. 13) with or without parenchymal involvement [15, 54, 91]. The presence of aortic root dilatation, ectopia lentis, dural ectasia, and musculoskeletal involvement favors the diagnosis [35, 96].
14-year-old with Marfan syndrome and headache, to rule out intracranial aneurysms. TOF-MRA (a) reveals marked tortuosity of the bilateral ICA with no definite intracranial aneurysms noted. Axial FLAIR image (b) shows associated focal infarction of posterior limb of left internal capsule and left thalamus (arrow)
Loeys-Dietz Syndrome:
Another AD disorder affecting the TGF‑β pathway with a triad of arterial abnormalities (tortuosity, aneurysm, and dissection), hypertelorism, and bifid uvula or cleft palate [35, 96].
COL Gene-related Disorder
COL3A1 Gene-related Type 4 (Vasculopathic) Ehlers-Danlos Syndrome:
An AD inherited disorder resulting from mutation of COL3A1 gene forming type III collagen [15, 35, 96]. CNS involvement may present with arterial dilatation, tortuosity, aneurysm, dissection, and caroticocavernous fistulas [35, 97]. Other distinctive features include skin translucency, extensive bruising, typical facies, and arterial or visceral rupture.
COL4A1/2 Gene-related Cerebral Disorder:
COL4A1/A2 gene mutation results in abnormal type IV collagen that provides vascular basement membrane scaffolding [35, 91, 98]. The CNS involvement can occur as early as in the antenatal period and up to adulthood [98]. The mutation of the COL4A1 gene presents as small vessel disease, while COL4A2 has a frequent stroke (hemorrhagic or ischemic) association [91]. Commonly encountered findings are unexplained white matter changes, porencephaly, and cerebral hemorrhage. The associated typical ophthalmologic findings and a positive family history help in diagnosis [91, 98].
Mimics
Reversible Cerebral Vasoconstriction Syndrome (RCVS):
A diverse group of entities characterized by reversible intracranial arterial vasospasm that can be multifocal, with or without associated parenchymal changes [15, 54]. RCVS is rare in children and shows male predilection, unlike adults [99, 100]. Arterial narrowing, subarachnoid hemorrhage, tiny scattered infarcts, and PRES-like appearance are the most frequent imaging findings [7, 15, 54]. Reversibility of angiographic findings within 12 weeks and the absence or subtle enhancement of the vessel wall help to differentiate it from cPACNS [18, 46, 89]. The multifocal nature is against the diagnosis of focal cerebral arteriopathy.
Arterial Dissection:
Craniocervical arterial dissection is uncommon in children and mostly idiopathic or occurs following trauma. Intracranial involvement is more common, with frequent anterior circulation involvement [101]. CT may show luminal narrowing and vessel expansion with a larger outer diameter, while MR may demonstrate crescentic intramural hematoma, best visualized on T1W images with fat suppression [54, 101].
Inflammatory Disorders:
Many inflammatory CNS disorders mimic angio-negative or small vessel vasculitis [5]. Demyelinating diseases (acute demyelinating encephalomyelitis, neuromyelitis optica, and MS) and autoimmune encephalitis (anti-NMDAR and limbic encephalitis) are the most important conditions that frequently present with white matter changes in the absence of vascular abnormalities [5]. Clinical, laboratory, and imaging findings can be inconclusive, and rarely histopathological confirmation may be required.
Clinical Radiological Approach
A child with suspected CCV requires a comprehensive clinical radiological evaluation (Table 3). In the diagnostic assessment of suspected CCV, the initial step is detailed history taking with thorough clinical examination and strong suspicion. The second step is performing relevant blood and CSF analyses to assess inflammatory biomarkers, to rule out pre-existing illnesses, metabolic causes, rheumatoid diseases, infections, or drugs. Evaluation for specific antibodies helps diagnose and exclude systemic vasculitis and autoimmune disorders. The crucial next step is imaging evaluation of the CNS and craniocervical vessels; MRI with MRA and VWI being the investigations of choice. CA may be performed as a problem solving tool in selected cases, especially when MRA and VWI are negative or equivocal with a high index of clinical suspicion. The final confirmatory step is meningocortical biopsy which is frequently needed in AN-cPACNS and close mimics.
Conclusion
CCV is a diverse group of disorders characterized by inflammation of the cerebral blood vessels due to myriad pathologies. They can present with typical or atypical imaging findings, posing a diagnostic challenge and requiring a strong clinical suspicion. The conventional and advanced imaging sequences are vital in identifying the salient features and diagnosing CCV, narrowing the differential diagnoses, and guiding appropriate management. Understanding and identifying genetic and non-inflammatory vasculopathies are quintessential as these are increasingly recognized with CCV. Despite the complexity, a stepwise approach can help arrive at an appropriate diagnosis and rule out common mimics.
References
Cellucci T, Benseler SM. Diagnosing central nervous system vasculitis in children. Curr Opin Pediatr. 2010;22:731–8.
Calabrese LH, Mallek JA. Primary angiitis of the central nervous system. Report of 8 new cases, review of the literature, and proposal for diagnostic criteria. Medicine (Baltimore). 1988;67:20–39.
Schnabel A, Hedrich CM. Childhood Vasculitis. Front Pediatr. 2019;6:421.
Hajj-Ali RA, Calabrese LH. Diagnosis and classification of central nervous system vasculitis. J Autoimmun. 2014;48-49:149–52.
Twilt M, Benseler SM. The spectrum of CNS vasculitis in children and adults. Nat Rev Rheumatol. 2011;8:97–107.
Sag E, Batu ED, Ozen S. Childhood systemic vasculitis. Best Pract Res Clin Rheumatol. 2017;31:558–75.
Berlit P, Kraemer M. Cerebral vasculitis in adults: what are the steps in order to establish the diagnosis? Red flags and pitfalls. Clin Exp Immunol. 2014;175:419–24.
Berlit P. Diagnosis and treatment of cerebral vasculitis. Ther Adv Neurol Disord. 2010;3:29–42.
Benseler SM, Silverman E, Aviv RI, Schneider R, Armstrong D, Tyrrell PN, deVeber G. Primary central nervous system vasculitis in children. Arthritis Rheum. 2006;54:1291–7.
Cellucci T, Tyrrell PN, Twilt M, Sheikh S, Benseler SM. Distinct phenotype clusters in childhood inflammatory brain diseases: implications for diagnostic evaluation. Arthritis Rheumatol. 2014;66:750–6.
Twilt M, Benseler SM. Treatment of CNS Vasculitis in Children. Curr Treat Options in Rheum. 2015;1:365–80.
Cellucci T, Tyrrell PN, Pullenayegum E, Benseler SM. von Willebrand factor antigen--a possible biomarker of disease activity in childhood central nervous system vasculitis? Rheumatology (Oxford). 2012;51:1838–45.
Hutchinson C, Elbers J, Halliday W, Branson H, Laughlin S, Armstrong D, Hawkins C, Westmacott R, Benseler SM. Treatment of small vessel primary CNS vasculitis in children: an open-label cohort study. Lancet Neurol. 2010;9:1078–84. Erratum in: Lancet Neurol. 2010;9:1045.
Abdel Razek AA, Alvarez H, Bagg S, Refaat S, Castillo M. Imaging spectrum of CNS vasculitis. Radiographics. 2014;34:873–94.
Soun JE, Song JW, Romero JM, Schaefer PW. Central Nervous System Vasculopathies. Radiol Clin North Am. 2019;57:1117–31.
Garg A. Vascular brain pathologies. Neuroimaging Clin N Am. 2011;21:897–926.
Bouhaouala MH, Charfi M, Saîd W, El Fourti S, Hendaoui L. Nervous system vasculitis. In: Hendaoui L, Stanson AW, Bouhaouala MH, Joffre F, editors. Systemic Vasculitis. Heidelberg: Springer; 2012. pp. 415–23. https://doi.org/10.1007/174_2011_240.
Aviv RI, Benseler SM, Silverman ED, Tyrrell PN, Deveber G, Tsang LM, Armstrong D. MR imaging and angiography of primary CNS vasculitis of childhood. AJNR Am J Neuroradiol. 2006;27:192–9.
Salvarani C, Brown RD Jr, Calamia KT, Christianson TJ, Weigand SD, Miller DV, Giannini C, Meschia JF, Huston J 3rd, Hunder GG. Primary central nervous system vasculitis: analysis of 101 patients. Ann Neurol. 2007;62:442–51.
Iannetti L, Zito R, Bruschi S, Papetti L, Ulgiati F, Nicita F, Del Balzo F, Spalice A. Recent understanding on diagnosis and management of central nervous system vasculitis in children. Clin Dev Immunol. 2012. https://doi.org/10.1155/2012/698327.
Swartz RH, Bhuta SS, Farb RI, Agid R, Willinsky RA, Terbrugge KG, Butany J, Wasserman BA, Johnstone DM, Silver FL, Mikulis DJ. Intracranial arterial wall imaging using high-resolution 3-tesla contrast-enhanced MRI. Neurology. 2009;72:627–34.
Hajj-Ali RA, Singhal AB, Benseler S, Molloy E, Calabrese LH. Primary angiitis of the CNS. Lancet Neurol. 2011;10:561–72.
Harris KG, Tran DD, Sickels WJ, Cornell SH, Yuh WT. Diagnosing intracranial vasculitis: the roles of MR and angiography. AJNR Am J Neuroradiol. 1994;15:317–30.
Birnbaum J, Hellmann DB. Primary angiitis of the central nervous system. Arch Neurol. 2009;66:704–9.
Mossa-Basha M, Shibata DK, Hallam DK, de Havenon A, Hippe DS, Becker KJ, Tirschwell DL, Hatsukami T, Balu N, Yuan C. Added Value of Vessel Wall Magnetic Resonance Imaging for Differentiation of Nonocclusive Intracranial Vasculopathies. Stroke. 2017;48:3026–33.
Lindenholz A, Harteveld AA, Zwanenburg JJM, Siero JCW, Hendrikse J. Comparison of 3T Intracranial Vessel Wall MRI Sequences. AJNR Am J Neuroradiol. 2018;39:1112–20.
Bhogal P, Navaei E, Makalanda HL, Brouwer PA, Sjöstrand C, Mandell DM, Lilja A. Intracranial vessel wall MRI. Clin Radiol. 2016;71:293–303.
Blumfield E, Moore MM, Drake MK, Goodman TR, Lewis KN, Meyer LT, Ngo TD, Sammet C, Stanescu AL, Swenson DW, Slovis TL, Iyer RS. Survey of gadolinium-based contrast agent utilization among the members of the Society for Pediatric Radiology: a Quality and Safety Committee report. Pediatr Radiol. 2017;47:665–73.
Eleftheriou D, Cox T, Saunders D, Klein NJ, Brogan PA, Ganesan V. Investigation of childhood central nervous system vasculitis: magnetic resonance angiography versus catheter cerebral angiography. Dev Med Child Neurol. 2010;52:863–7.
John S, Hajj-Ali RA. CNS vasculitis. Semin Neurol. 2014;34:405–12.
Elbers J, Halliday W, Hawkins C, Hutchinson C, Benseler SM. Brain biopsy in children with primary small-vessel central nervous system vasculitis. Ann Neurol. 2010;68:602–10.
Venkateswaran S, Hawkins C, Wassmer E. Diagnostic yield of brain biopsies in children presenting to neurology. J Child Neurol. 2008;23:253–8.
Zhou Q, Yang D, Ombrello AK, Zavialov AV, Toro C, Zavialov AV, Stone DL, Chae JJ, Rosenzweig SD, Bishop K, Barron KS, Kuehn HS, Hoffmann P, Negro A, Tsai WL, Cowen EW, Pei W, Milner JD, Silvin C, Heller T, Chin DT, Patronas NJ, Barber JS, Lee CC, Wood GM, Ling A, Kelly SJ, Kleiner DE, Mullikin JC, Ganson NJ, Kong HH, Hambleton S, Candotti F, Quezado MM, Calvo KR, Alao H, Barham BK, Jones A, Meschia JF, Worrall BB, Kasner SE, Rich SS, Goldbach-Mansky R, Abinun M, Chalom E, Gotte AC, Punaro M, Pascual V, Verbsky JW, Torgerson TR, Singer NG, Gershon TR, Ozen S, Karadag O, Fleisher TA, Remmers EF, Burgess SM, Moir SL, Gadina M, Sood R, Hershfield MS, Boehm M, Kastner DL, Aksentijevich I. Early-onset stroke and vasculopathy associated with mutations in ADA2. N Engl J Med. 2014;370:911–20.
Ramantani G, Niggemann P, Bast T, Lee-Kirsch MA. Reconciling neuroimaging and clinical findings in Aicardi-Goutières syndrome: an autoimmune-mediated encephalopathy. AJNR Am J Neuroradiol. 2010;31:E62-3; author reply E64.
Watts RA, Conaghan PG, Denton C, Foster H, Isaacs J, Müller-Ladner U. Oxford textbook of rheumatology. 4. ed. Oxford: OUP; 2013.
Smitka M, Bruck N, Engellandt K, Hahn G, Knoefler R, von der Hagen M. Clinical Perspective on Primary Angiitis of the Central Nervous System in Childhood (cPACNS). Front Pediatr. 2020;8:281.
Gowdie P, Twilt M, Benseler SM. Primary and secondary central nervous system vasculitis. J Child Neurol. 2012;27:1448–59.
Cravioto H, Feigin I. Noninfectious granulomatous angiitis with a predilection for the nervous system. Neurology. 1959;9:599–609.
Matsell DG, Keene DL, Jimenez C, Humphreys P. Isolated angiitis of the central nervous system in childhood. Can J Neurol Sci. 1990;17:151–4.
Twilt M, Benseler SM. Central nervous system vasculitis in adults and children. Handb Clin Neurol. 2016;133:283–300.
Gallagher KT, Shaham B, Reiff A, Tournay A, Villablanca JP, Curran J, Nelson MD Jr, Bernstein B, Rawlings DJ. Primary angiitis of the central nervous system in children: 5 cases. J Rheumatol. 2001;28:616–23.
Amlie-Lefond C, Bernard TJ, Sébire G, Friedman NR, Heyer GL, Lerner NB, DeVeber G, Fullerton HJ; International Pediatric Stroke Study Group. Predictors of cerebral arteriopathy in children with arterial ischemic stroke: results of the International Pediatric Stroke Study. Circulation. 2009;119:1417–23.
Braun KP, Bulder MM, Chabrier S, Kirkham FJ, Uiterwaal CS, Tardieu M, Sébire G. The course and outcome of unilateral intracranial arteriopathy in 79 children with ischaemic stroke. Brain. 2009;132:544–57.
Aviv RI, Benseler SM, DeVeber G, Silverman ED, Tyrrell PN, Tsang LM, Armstrong D. Angiography of primary central nervous system angiitis of childhood: conventional angiography versus magnetic resonance angiography at presentation. AJNR Am J Neuroradiol. 2007;28:9–15.
Salvarani C, Brown RD Jr, Calamia KT, Christianson TJ, Huston J 3rd, Meschia JF, Giannini C, Miller DV, Hunder GG. Primary CNS vasculitis with spinal cord involvement. Neurology. 2008;70:2394–400.
Küker W, Gaertner S, Nagele T, Dopfer C, Schoning M, Fiehler J, Rothwell PM, Herrlinger U. Vessel wall contrast enhancement: a diagnostic sign of cerebral vasculitis. Cerebrovasc Dis. 2008;26:23–9.
Benseler SM, deVeber G, Hawkins C, Schneider R, Tyrrell PN, Aviv RI, Armstrong D, Laxer RM, Silverman ED. Angiography-negative primary central nervous system vasculitis in children: a newly recognized inflammatory central nervous system disease. Arthritis Rheum. 2005;52:2159–67.
Lie JT. Primary (granulomatous) angiitis of the central nervous system: a clinicopathologic analysis of 15 new cases and a review of the literature. Hum Pathol. 1992;23:164–71.
Batthish M, Banwell B, Laughlin S, Halliday W, Peschken C, Paras E, Benseler S. Refractory primary central nervous system vasculitis of childhood: successful treatment with infliximab. J Rheumatol. 2012;39:2227–9.
Beelen J, Benseler SM, Dropol A, Ghali B, Twilt M. Strategies for treatment of childhood primary angiitis of the central nervous system. Neurol Neuroimmunol Neuroinflamm. 2019;6:e567.
Chenevier F, Renoux C, Marignier R, Durand-Dubief F, Hermier M, Streichenberger N, Vukusic S, Confavreux C. Primary angiitis of the central nervous system: response to mycophenolate mofetil. J Neurol Neurosurg Psychiatry. 2009;80:1159–61.
Ford-Jones EL, Macgregor D, Richardson S, Jamieson F, Blaser S, Artsob H. Acute childhood encephalitis and meningoencephalitis: Diagnosis and management. Paediatr Child Health. 1998;3:33–40.
Rodríguez-Pla A, Stone JH. Vasculitis and systemic infections. Curr Opin Rheumatol. 2006;18:39–47.
Agarwal A, Bathla G, Kanekar S. Imaging of Non-atherosclerotic Vasculopathies. J Clin Imaging Sci. 2020;10:62.
Mohan S, Jain KK, Arabi M, Shah GV. Imaging of meningitis and ventriculitis. Neuroimaging Clin N Am. 2012;22:557–83.
Lanthier S, Armstrong D, Domi T, deVeber G. Post-varicella arteriopathy of childhood: natural history of vascular stenosis. Neurology. 2005;64:660–3.
Askalan R, Laughlin S, Mayank S, Chan A, MacGregor D, Andrew M, Curtis R, Meaney B, deVeber G. Chickenpox and stroke in childhood: a study of frequency and causation. Stroke. 2001;32:1257–62.
Derin S, Derin H, Sahan M, Caksen H. A pediatric case of ramsay hunt syndrome. Case Rep Otolaryngol. 2014;2014:469565.
Lindström J, Grahn A, Zetterberg H, Studahl M. Cerebrospinal fluid viral load and biomarkers of neuronal and glial cells in Ramsay Hunt syndrome. Eur J Neurosci. 2016;44:2944–9.
Patsalides AD, Wood LV, Atac GK, Sandifer E, Butman JA, Patronas NJ. Cerebrovascular disease in HIV-infected pediatric patients: neuroimaging findings. AJR Am J Roentgenol. 2002;179:999–1003.
Hoang A, Chorath K, Moreira A, Evans M, Burmeister-Morton F, Burmeister F, Naqvi R, Petershack M, Moreira A. COVID-19 in 7780 pediatric patients: a systematic review. EClinicalMedicine. 2020;24:00433. http://www.thelancet.com/journals/eclinm/article/PIIS2589-5370(20)30177-2/abstract. Accessed 8 May 2021.
Khanna G, Sargar K, Baszis KW. Pediatric vasculitis: recognizing multisystemic manifestations at body imaging. Radiographics. 2015;35:849–65.
Barut K, Şahin S, Adroviç A, Kasapçopur Ö. Diagnostic approach and current treatment options in childhood vasculitis. Turk Pediatri Ars. 2015;50:194–205.
Russo RAG, Katsicas MM. Takayasu Arteritis. Front Pediatr. 2018;6:265.
Cakar N, Yalcinkaya F, Duzova A, Caliskan S, Sirin A, Oner A, Baskin E, Bek K, Soylu A, Fitoz S, Bayazit AK, Bircan Z, Ozen S, Uncu N, Ekim M. Takayasu arteritis in children. J Rheumatol. 2008;35:913–9.
Singh N, Hughes M, Sebire N, Brogan P. Takayasu arteritis in infancy. Rheumatology (Oxford). 2013;52:2093–5.
Gotway MB, Araoz PA, Macedo TA, Stanson AW, Higgins CB, Ring EJ, Dawn SK, Webb WR, Leung JW, Reddy GP. Imaging findings in Takayasu’s arteritis. AJR Am J Roentgenol. 2005;184:1945–50.
Alves NR, Magalhães CM, Almeida Rde F, Santos RC, Gandolfi L, Pratesi R. Prospective study of Kawasaki disease complications: review of 115 cases. Rev Assoc Med Bras (1992). 2011;57:295–300.
Okanishi T, Enoki H. Transient subcortical high-signal lesions in Kawasaki syndrome. Pediatr Neurol. 2012;47:295–8.
Stojanovic V, Radovanović T, Koprivšek K, Vijatov Ðurić G, Doronjski A. Kawasaki disease complicated with cerebral vasculitis and severe encephalitis. Ann Indian Acad Neurol. 2020;23:228–32.
Navon Elkan P, Pierce SB, Segel R, Walsh T, Barash J, Padeh S, Zlotogorski A, Berkun Y, Press JJ, Mukamel M, Voth I, Hashkes PJ, Harel L, Hoffer V, Ling E, Yalcinkaya F, Kasapcopur O, Lee MK, Klevit RE, Renbaum P, Weinberg-Shukron A, Sener EF, Schormair B, Zeligson S, Marek-Yagel D, Strom TM, Shohat M, Singer A, Rubinow A, Pras E, Winkelmann J, Tekin M, Anikster Y, King MC, Levy-Lahad E. Mutant adenosine deaminase 2 in a polyarteritis nodosa vasculopathy. N Engl J Med. 2014;370:921–31.
Santhanam S, Thambithurai R, Palaniappan N, Vij M, Kalyanasundaram S. Childhood polyarteritis nodosa presenting as central nervous system vasculitis. Indian J Rheumatol . 2019;14:4–6.
Ozen S, Pistorio A, Iusan SM, Bakkaloglu A, Herlin T, Brik R, Buoncompagni A, Lazar C, Bilge I, Uziel Y, Rigante D, Cantarini L, Hilario MO, Silva CA, Alegria M, Norambuena X, Belot A, Berkun Y, Estrella AI, Olivieri AN, Alpigiani MG, Rumba I, Sztajnbok F, Tambic-Bukovac L, Breda L, Al-Mayouf S, Mihaylova D, Chasnyk V, Sengler C, Klein-Gitelman M, Djeddi D, Nuno L, Pruunsild C, Brunner J, Kondi A, Pagava K, Pederzoli S, Martini A, Ruperto N; Paediatric Rheumatology International Trials Organisation (PRINTO). EULAR/PRINTO/PRES criteria for Henoch-Schönlein purpura, childhood polyarteritis nodosa, childhood Wegener granulomatosis and childhood Takayasu arteritis: Ankara 2008. Part II: Final classification criteria. Ann Rheum Dis. 2010;69:798–806.
Zheng Y, Zhang Y, Cai M, Lai N, Chen Z, Ding M. Central Nervous System Involvement in ANCA-Associated Vasculitis: What Neurologists Need to Know. Front Neurol. 2019;9:1166.
Pakalniskis MG, Berg AD, Policeni BA, Gentry LR, Sato Y, Moritani T, Smoker WR. The Many Faces of Granulomatosis With Polyangiitis: A Review of the Head and Neck Imaging Manifestations. AJR Am J Roentgenol. 2015;205:W619–29.
Vodopivec I, Lobo AM, Prasad S. Ocular inflammation in neurorheumatic disease. Semin Neurol. 2014;34:444–57.
Bhadu D, Kumar P, Malhotra KP, Sharma A, Sharma M, Srivastava D. Central nervous system vasculitis in pediatric microscopic polyangiitis. Acta Reumatol Port. 2016;41:372–5.
Pacheva IH, Ivanov IS, Stefanova K, et al. Central Nervous System Involvement in Henoch-Schonlein Purpura in Children and Adolescents. Case Rep Pediatr. 2017. https://doi.org/10.1155/2017/5483543.
Topcuoglu OM, Topcuoglu ED, Altay CM, Genc S. Imaging pearls of pediatric Behçet’s disease. Eur J Radiol. 2017;94:115–24.
Yıldız M, Köker O, Adrovic A, Şahin S, Barut K, Kasapçopur Ö. Pediatric Behçet’s disease - clinical aspects and current concepts. Eur J Rheumatol. 2019;7(Suppl 1):1–10. https://doi.org/10.5152/eurjrheum.2019.19121.
Metreau-Vastel J, Mikaeloff Y, Tardieu M, Koné-Paut I, Tran TA. Neurological involvement in paediatric Behçet’s disease. Neuropediatrics. 2010;41:228–34.
Smith EMD, Lythgoe H, Hedrich CM. Vasculitis in Juvenile-Onset Systemic Lupus Erythematosus. Front Pediatr. 2019;7:149.
Li SC. Scleroderma in Children and Adolescents: Localized Scleroderma and Systemic Sclerosis. Pediatr Clin North Am. 2018;65:757–81.
Soliotis FC, Mavragani CP, Moutsopoulos HM. Central nervous system involvement in Sjogren’s syndrome. Ann Rheum Dis. 2004;63:616–20.
Elst EF, Kamphuis SS, Prakken BJ, Wulffraat NM, van der Net J, Peters AC, Kuis W. Case report: severe central nervous system involvement in juvenile dermatomyositis. J Rheumatol. 2003;30:2059–63.
Papadopoulou C, McCann LJ. The Vasculopathy of Juvenile Dermatomyositis. Front Pediatr. 2018;6:284.
Dolapcioglu C, Dolapcioglu H. Structural brain lesions in inflammatory bowel disease. World J Gastrointest Pathophysiol. 2015;6:124–30.
Ma W, Li XJ, Li W, Xiao L, Ji XJ, Xu Y. MRI findings of central nervous system involvement in children with haemophagocytic lymphohistiocytosis: correlation with clinical biochemical tests. Clin Radiol. 2021;76:159.e9–17.
Malik P, Antonini L, Mannam P, Aboobacker FN, Merve A, Gilmour K, Rao K, Kumar S, Mani SE, Eleftheriou D, Rao A, Hemingway C, Sudhakar SV, Bartram J, Mankad K. MRI Patterns in Pediatric CNS Hemophagocytic Lymphohistiocytosis. AJNR Am J Neuroradiol. 2021;42:2077–85.
Bonardi M, Turpini E, Sanfilippo G, Mina T, Tolva A, Zappoli Thyrion F. Brain Imaging Findings and Neurologic Complications after Allogenic Hematopoietic Stem Cell Transplantation in Children. Radiographics. 2018;38:1223–38.
McCrea N, Fullerton HJ, Ganesan V. Genetic and Environmental Associations With Pediatric Cerebral Arteriopathy. Stroke. 2019;50:257–65.
Amans MR, Stout C, Fox C, Narvid J, Hetts SW, Cooke DL, Higashida RT, Dowd CF, McSwain H, Halbach VV. Cerebral arteriopathy associated with Arg179His ACTA2 mutation. BMJ Case Rep. 2013;2013:bcr2013010997.
D’Arco F, Alves CA, Raybaud C, Chong WKK, Ishak GE, Ramji S, Grima M, Barkovich AJ, Ganesan V. Expanding the Distinctive Neuroimaging Phenotype of ACTA2 Mutations. AJNR Am J Neuroradiol. 2018;39:2126–31.
Abdel-Salam GMH, Abdel-Hamid MS, Mohammad SA, Abdel-Ghafar SF, Soliman DR, El-Bassyouni HT, Effat L, Zaki MS. Aicardi-Goutières syndrome: unusual neuro-radiological manifestations. Metab Brain Dis. 2017;32:679–83.
Kirton A, Crone M, Benseler S, Mineyko A, Armstrong D, Wade A, Sebire G, Crous-Tsanaclis AM, deVeber G. Fibromuscular dysplasia and childhood stroke. Brain. 2013;136:1846–56.
Kim ST, Brinjikji W, Lanzino G, Kallmes DF. Neurovascular manifestations of connective-tissue diseases: A review. Interv Neuroradiol. 2016;22:624–37.
Byers PH. Vascular Ehlers-Danlos syndrome. In: Adam MP, Ardinger HH, Pagon RA, Wallace SE, Bean LJ, Mirzaa G, et al., editors. GeneReviews. Seattle: University of Washington; 1993. http://www.ncbi.nlm.nih.gov/books/NBK1494/.
Shah S, Ellard S, Kneen R, Lim M, Osborne N, Rankin J, Stoodley N, van der Knaap M, Whitney A, Jardine P. Childhood presentation of COL4A1 mutations. Dev Med Child Neurol. 2012;54:569–74.
Coffino SW, Fryer RH. Reversible Cerebral Vasoconstriction Syndrome in Pediatrics: A Case Series and Review. J Child Neurol. 2017;32:614–23.
Durrleman C, Naggara O, Grevent D, Belot A, Desgranges M, Boyer O, Chabrier S, Bader-Meunier B, Kossorotoff M. Reversible cerebral vasoconstriction syndrome in paediatric patients with systemic lupus erythematosus: implications for management. Dev Med Child Neurol. 2019;61:725–9.
Rafay MF, Armstrong D, Deveber G, Domi T, Chan A, MacGregor DL. Craniocervical arterial dissection in children: clinical and radiographic presentation and outcome. J Child Neurol. 2006;21:8–16.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
N. Gupta, S.B. Hiremath, R.I. Aviv, and N. Wilson declare that they have no competing interests.
Rights and permissions
About this article
Cite this article
Gupta, N., Hiremath, S.B., Aviv, R.I. et al. Childhood Cerebral Vasculitis. Clin Neuroradiol 33, 5–20 (2023). https://doi.org/10.1007/s00062-022-01185-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00062-022-01185-8