Abstract
Introduction
The clinical and MR imaging features of neurosyphilis are highly varied. In this study, we describe the spectrum of the imaging findings in patients with neurosyphilis.
Methods
The MR imaging observations of 35 patients diagnosed to have neurosyphilis on the basis of cerebrospinal fluid reactive for the Venereal Disease Research Laboratory test were reviewed.
Results
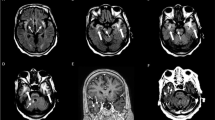
All the 35 patients, including four with human immunodeficiency virus coinfection, met the CDC diagnostic criteria for neurosyphilis. Patients were classified into three groups: (1) neuropsychiatric, (2) meningovascular, and (3) myelopathic, based on the dominant clinical manifestations. Fourteen patients with neuropsychiatric manifestations showed diffuse cerebral atrophy (14), parenchymal signal changes in the mesial temporal region (2) and temporal and basifrontal regions (1), infarcts (3), and nonspecific white matter changes (3). Eleven patients with meningovascular form showed infarcts (6), diffuse cerebral atrophy (3), signal changes in the mesial temporal region (3), sulcal exudates (1), progressive multifocal leukoencephalopathy (1), and a mass surrounding the carotid sheath (1). Spine imaging in ten patients with myelopathy showed long-segment signal changes (5), contrast enhancement (2), and dorsal column involvement (2). Three of these patients had normal spinal study. Six patients in the myelopathic group also underwent brain MRI that showed signal changes in the temporal region (2) and frontal region (1), multiple infarcts (1), and enhancing hypothalami (1). Three patients had normal study.
Conclusion
MRI abnormalities in neurosyphilis are protean and mimic of many other neurological disorders and thus require a high index of suspicion to reduce diagnostic omissions.




Similar content being viewed by others
References
Tien RD, Gean-Marton AD, Mark AS (1992) Neurosyphilis in HIV carriers: MR findings in six patients. Am J Roentgenol 158:1325–1328
Brightbill TC, Ihmeidan IH, Post MJD, Berger JR, Katz DA (1995) Neurosyphilis in HIV-positive and HIV-negative patients: neuroimaging findings. Am J Neuroradiol 16:703–711
Zifko U, Wimberger D, Lindner K, Zier G, Grisold W, Schindler E (1996) MRI in patients with general paresis. Neuroradiology 38:120–123
Srivastava T, Thussu A (2000) MRI in syphilitic meningomyelitis. Neurol India 48:196–197
Nabatame H, Nakamura K, Matuda M, Fujimoto N, Dodo Y, Imura T (1992) MRI of syphilitic myelitis. Neuroradiology 34:105–106
Chilver-Stainer L, Fischer U, Hauf M, Fux CA, Sturzenegger M (2009) Syphilitic myelitis: rare, nonspecific, but treatable. Neurology 72:673–675
Centers for Disease Control and Prevention, (2000) Summary of notifiable diseases—United States. MMWR Morb Mortal Wkly Rep 49:83
Timmermann M, Carr J (2004) Neurosyphilis in the modern era. J Neurol Neurosurg Psychiatry 75:1727–1730
Holland BA, Perrett LV, Mills CM (1986) Meningovascular syphilis: CT and MR findings. Radiology 158:439–442
Gurses C, Bilgic B, Topcular B et al (2007) Clinical and magnetic resonance imaging findings of HIV-negative patients with neurosyphilis. J Neurol 254:368
Russouw HG, Roberts MC, Emsley RA, Truter R (1997) Psychiatric manifestations and magnetic resonance imaging in HIV-negative neurosyphilis. Biol Psychiatry 41:467–473
Bash S, Hathout GM, Cohen S (2001) Mesiotemporal T2-weighted hyperintensity: neurosyphilis mimicking herpes encephalitis. Am J Neuroradiol 22:314–316
Santos VA, Matias S, Saraiva P, Goulao A (2005) Differential diagnosis of mesiotemporal lesions: case report of neurosyphilis. Neuroradiology 47:664–667
Sinha S, Harish T, Taly AB, Murthy P, Nagarathna S, Chandramuki A (2008) Symptomatic seizures in neurosyphilis: an experience from a university hospital in south India. Seizure 17:711–716
Yingxin Y, Mengqi W, Yuangui H et al (2010) Clinical presentation and imaging of general paresis due to neurosyphilis in patients negative for human immunodeficiency virus. J Clin Neurosci 17:308–310
Gállego J, Soriano G, Zubieta JL, Delgado G, Villanueva JA (1994) Magnetic resonance angiography in meningovascular syphilis. Neuroradiology 36:208–209
Berger JR (1992) Spinal cord syphilis associated with human immunodeficiency virus infection: a treatable myelopathy. Am J Med 92:101–103
Tashiro K, Moriwaka F, Sudo K, Akino M, Abe H (1987) Syphilitic myelitis with its magnetic resonance imaging (MRI) verification and successful treatment. J Psychiatry Neurol 41:269–271
Kikuchi S, Shinpo K, Niino M, Tashiro K (2003) Subacute syphilitic meningomyelitis with characteristic spinal MRI findings. J Neurol 250:106–107
Berger JR, Harris JO, Gregarios J, Norenberg M (1990) Cerebrovascular disease in AIDS: a case control study. AIDS 4:239–244
Alam F, Yasutomi H, Fukuda H et al (2006) Diffuse cerebral white matter T2-weighted hyperintensity: a new finding of general paresis. Acta Radiol 47:609–611
Johns DR, Tierney M, Felsenstein D (1987) Alteration in the natural history of neurosyphilis by concurrent infection with the human immunodeficiency virus. N Engl J Med 316:1569–1572
Katz DA, Berger JR, Duncan RC (1993) Neurosyphilis: a comparative study of the effects of infection with human immunodeficiency virus. Arch Neurol 50:243–249
Conflict of interest
We declare that we have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Nagappa, M., Sinha, S., Taly, A.B. et al. Neurosyphilis: MRI features and their phenotypic correlation in a cohort of 35 patients from a tertiary care university hospital. Neuroradiology 55, 379–388 (2013). https://doi.org/10.1007/s00234-012-1017-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-012-1017-9