Indications
Urgent
Meningitis 1
- It is very difficult to clinically rule out meningitis with out an LP. Fever, neck stiffness, altered mental status, and headache are the most common symptoms.
- Only 2 effective ways to rule out meningitis
- Jolt Acceleration
- Sensitivity 97% Specificity 60%
- Patient turns their head horizontally 2 rotations a second for several seconds. If this does not worsen their headache, then you can rule out meningitis.
- Absence of fever, headache, AND altered mental status
- Sensitivity 99%
- If any one of these three are present you cannot rule out meningitis
- Jolt Acceleration
Subarachnoid Hemorrhage
- For a thunderclap headache and a negative head CT, an LP should be performed to look for xanthochromia
Non-urgent
- Wide variety of indications including suspicion for multiple sclerosis, guillain barre, paraneoplastic antibodies, leptomeningeal carcinomatosis, normal pressure hydrocephalus, pseudotumor cerebri
Contraindications
Increased Intracranial Pressure
- IDSA recommends head CT prior to LP if2
- Immunosuppressed
- History of stroke or CNS mass
- New onset seizure
- Altered mental status
- Focal neurologic deficits
- Papilledema

- If suspecting bacterial meningitis but need a CT, work up the patient in this order
- Blood cultures -> Antibiotics + Dexamethasone -> CT -> LP
- Meningococcal CSF cultures are often (-) 1 hour after antibiotics, but strep pneumonia CSF will remain (+) 4 hours after antibiotics 3
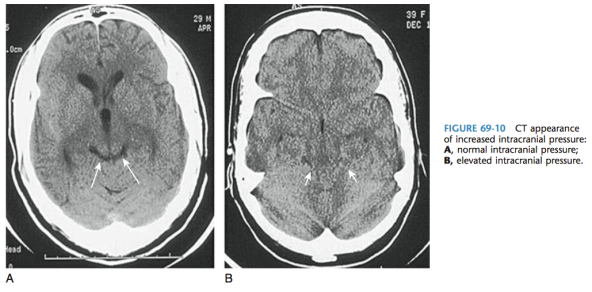
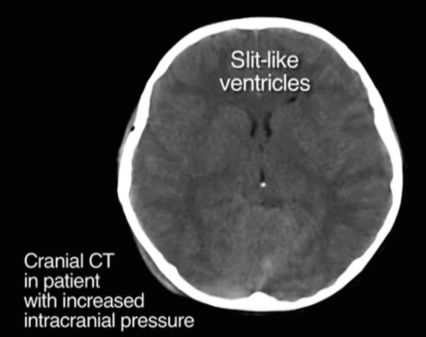
- Concerning CT findings include4
- Midline shift
- Loss of normal cisterns and ventricles
- Ask yourself: are there any black fluid filled spaces in the brain that are missing on this CT?
Hyper-dense subdural hematoma causing midline shift and compression of the lateral ventricle.
Risk of bleeding
- Goal platelets > 50,000 5
- No risk of bleeding has been seen with aspirin
- Plavix and other anti-platelet medications have not been studied
- Goal INR < 1.5 6
- Therapeutic anticoagulation increases the incidence of spinal hematoma and paraparesis to an absolute risk of 2%
- Therapeutic anticoagulation should be avoided
- Delay non-urgent LP’s 12-24 hours after prophylactic anticoagulation
Cardiorespiratory Compromise
- Consider how patient positioning could jeopardize the patients breathing or volume status
Infection at the site of needle insertion
- Cellulitis
- Epidural abscess
Next Page: Complications
References
1. Attia, J., Hatala, R., Cook, D.J. & Wong, J.G. DOes this adult patient have acute meningitis? JAMA 282, 175-181 (1999).
2. Tunkel, A.R. et al. Practice Guidelines for the Management of Bacterial Meningitis. Clinical Infectious Diseases 39, 1267-1284 (2004).
3. Kanegaye, J.T., Soliemanzadeh, P. & Bradley, J.S. Lumbar puncture in pediatric bacterial meningitis: defining the time interval for recovery of cerebrospinal fluid pathogens after parenteral antibiotic pretreatment. Pediatrics 108, 1169-74 (2001).
4. Joffe, A.R. Lumbar puncture and brain herniation in acute bacterial meningitis: a review. J Intensive Care Med 22, 194-207 (2007).
5. Vavricka, S.R., Walter, R.B., Irani, S., Halter, J. & Schanz, U. Safety of lumbar puncture for adults with acute leukemia and restrictive prophylactic platelet transfusion. Ann Hematol 82, 570-3 (2003).
6. Ruff, R.L. & Dougherty, J.H., Jr. Complications of lumbar puncture followed by anticoagulation. Stroke 12, 879-81 (1981).