It is often stated that the human foot has 3 arches; two longitudinal arches and the transverse arch (sometimes also referred to as the metatarsal arch).1 Whereas the presence of longitudinal arches are unanimously accepted, the transverse metatarsal arch of the foot is considered to be quite controversial. Believe it or not its existence has been debated since last century. But what is the transverse metatarsal arch? And what does the research actually tell us about it?
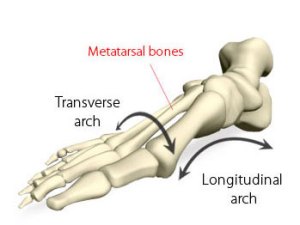
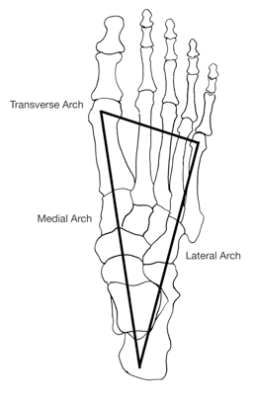
The existence of a transverse arch at the metatarsal region would require the pressure to be greatest at the areas beneath the 1st and 5th metatarsal heads, and the area of the 2nd, 3rd and 4th metatarsal heads to be elevated relative to this. This gives us the ‘tripod’ like weight distribution of the foot which was first described by Kapandji in 1970.2 However, the first descriptions of the transverse metatarsal arch date back as far as 100 years prior to Kapandji’s work3 and several papers published in Germany between 1882 and 1927 actually concluded that no transverse arch of the foot was usually present.4-7 Much of the research produced following Kapandji’s work concurs with these conclusions regarding the transverse metatarsal arch being a misnomer.
So if the presence of a transverse metatarsal arch has long been questioned, why have so many authors, and indeed medical professionals, subscribed to this theory for so long (and continue to do so) in spite of growing evidence against it?
The conception of the foot bearing its weight on three points must be quite attractive in order to persist (Jones, 1941)8
When a patient presents with diffuse pain across the forefoot, what should be performed is thorough examination of the region, identification of the anatomical structure which is involved, and then a management plan directed towards reducing the symptoms with the most appropriate treatment available. However, all too often a clinician will diagnose ‘metatarsalgia’ (NOT a diagnosis, but we’ll save that for another blog) caused by ‘dropped metatarsals’ or ‘a fallen metatarsal arch’. It’s very quick and very easy, and you can see how it doesn’t require too much thinking. For these clinicians to accept that a transverse metatarsal arch does not exist would require them to change their entire clinical practice, and for many this sort of paradigm shift in thinking is too uncomfortable to accept, so instead they continue as they are.
So, 100 year old journal articles written in German aside, lets look at some of the more current research which has looked at the mythical transverse metatarsal arch.
In 1997, Daentzer et al.9 performed a study on 100 feet. The age range of the participants in the study was between 10-72 years old. None of the participants had any foot deformity or symptoms. Ultrasonography was performed at the level of the metatarsal heads in both non weight bearing and weightbearing. Barefoot plantar pressure measurements were recorded using a force plate. Their findings/conclusions: Pressures are usually highest underneath the 2nd, 3rd and 4th metatarsal heads, there is no transverse metatarsal arch, and the forefoot is normally flat at the level of the metatarsal heads.
In 1999, Luger et al.10 performed a study on 720 feet (the largest study to my knowledge). The age range of the participants in the study was 18-83 years old. Interestingly they included individuals with a variety of foot symptoms and abnormalities as well as pain free individuals. The all had static and dynamic barefoot pressure measurements taken. Their findings/conclusions: Only 22 feet out of 720 (3%) had a dynamic metatarsal arch whilst walking, and this was only found in the feet classified as having deformity or pain. Not only was a transverse metatarsal arch rarely seen, but they concluded that it actually indicated a possible pathological deformity (i.e it is an abnormality which may cause problems)
In 2003, Kanatli et al.11 performed a study on 32 feet. The age range of the participants in the study was 20-30 years old. All participants were pain free and had no foot deformities. Barefoot plantar pressure measurements were taken whilst walking. Their findings/conclusions: Significantly higher pressures were recorded beneath the 2nd and 3rd metatarsal heads, and the transverse metatarsal arch did not exist in normal subjects.
 As you can see one of the common findings seen in the research discussed has been that higher pressures are not seen beneath the 1st and 5th metatarsal heads during gait. Other authors have investigated this employing pressure measurement equipment and found that the pressures in the middle metatarsals are consistently greater than the 1st and 5th metatarsals.12,13 All of the research suggests that the tripod configuration of the foot is completely erroneous, and without this, it is obvious that it is not possible for there to be a transverse metatarsal arch. Clinicians who continue to talk about the transverse arch, and offer treatments for its ‘collapse’ are either uninformed, bogged down in old habits or in denial.
As you can see one of the common findings seen in the research discussed has been that higher pressures are not seen beneath the 1st and 5th metatarsal heads during gait. Other authors have investigated this employing pressure measurement equipment and found that the pressures in the middle metatarsals are consistently greater than the 1st and 5th metatarsals.12,13 All of the research suggests that the tripod configuration of the foot is completely erroneous, and without this, it is obvious that it is not possible for there to be a transverse metatarsal arch. Clinicians who continue to talk about the transverse arch, and offer treatments for its ‘collapse’ are either uninformed, bogged down in old habits or in denial.
References
- Williams, P.L. et al. (1995) Gray’s Anatomy. 38th Edition, Churchill Livingstone, New York.
- Kapandji, L.A. (1970) The Physiology of the Joints. E & S Livingstone, Edinburgh.
- Henle, J. (1871) Handbuch der Knochenlehre des Menschen. Vieweg, Braunschweig.
- Beely, F. (1882) Zur Mechanik des Stehens. Uber die Bedeutung des Fussgewolbes im Stehen. Arch klin Chir, 27: 457-471.
- Momburg, F.A. (1909) Die Stutzpunkte des Fusses beim Gehen und Stehen. Dtsch med Wschr, 4: 148-152.
- Frostell, G. (1925) Beitrag zur Kenntnis der vorderen Stutzpunkte des Fusses, sowie des Fusswinkels beim Stehen und Gehen. Z Orthop Chir, 47: 3-54.
- Abramson, E. (1927) Zur Kenntnis der Mechanik des Mittelfusses. Skand Arch Physiol, 51: 175-234.
- Jones, R.L. (1941) The Human Foot. An experimental study of its mechanics, and the role of its muscles and ligaments in support of the arch. American Journal of Anatomy, 68: 1-39.
- Daentzer, D., Wulker, N., & Zimmermann, U. (1997) Observations concerning the transverse metatarsal arch. Foot and Ankle Surgery, 3: 15-20.
- Luger, E.J., Nissan, M., Karpf, A., Steinberg, E.L., & Dekel, S. (1999) Patterns of weight distribution under the metatarsal heads. The Journal of Bone & Joint Surgery (Br), 81: 199-202.
- Kanatli, U., Yetkin, H., & Bolukbasi, S. (2003) Evaluation of the transverse metatarsal arch of the foot with gait analysis. Arch Orthop Trauma Surg, 123: 148-150.
- Cavanagh, P.R., Rodgers, M.M., & Iiboshi, A. (1987) Pressure distribution under symptom-free feet during barefoot standing. Foot and Ankle, 7: 262-276.
- Hennig, E.M., & Milani, T.L. (1993) Die Dreipunktuntersttzung des Fusses. Eine Druckverteilungsanalyse bei statischer und dynamischer Belastung. Z Orthop, 131: 279-284.
Thank you forn this very interesting article!
Can you explain then why metatarsal pads work or why people experience “dropped metatarsals” where they can feel a marble-type bone when they walk? These situations imply that an arch exists- the pads to restore the arch and the “dropped” metatarsal having dropped down from above.
Please note, I am not trying to argue I just want to understand.
Thank you.
Hi Catherine,
Thanks for your comment. Can I explain why metatarsal pads work? Yes I can. They are issued by many for forefoot discomfort (of varying causes). Any modification such as a met pad/dome will alter the way the forefoot is loaded (the timing, magnitude and location of force acting beneath the forefoot). A met pad will also usually encourage 1st ray plantarflexion, which will in turn lower the force required to initiate the windlass mechanism and promote better forefoot mechanics. Either of these aforementioned mechanisms would potentially alter symptoms in the forefoot region… without restoring a fictional arch 😉
[I have made the assumption you are a healthcare professional – hence the language I have used. Apologies if I have jumped to conclusions.]
Regarding your second point, it is important to evaluate an assumption that your question is based on; Do people actually experience ‘dropped metatarsals’? Or are they just told they do? How can a specialist diagnose dropped metatarsals in a patient when they have probably never seen that patient before? (i.e. how do they know what they were like before??) Once again an overused, lazy (and probably bogus) diagnosis when confronted with forefoot pain in my opinion. Most individuals who experience feelings of walking on marbles/stones are indeed often walking on their metatarsal heads, but as a result of plantar metatarsal fat pad atrophy (or its anterior displacement) and not due to the metatarsals themselves having ‘dropped’.
Hope this answers your queries?
You may also find this quite an interesting read on the subject: http://www.podiatry-arena.com/podiatry-forum/showthread.php?t=339
Sir
For several months I have had a variable pain over the middle of my right dorsal metacarpals 2 and 3. Some slight soft swelling but otherwise no gross symptoms.
At times this is very painful to touch and is starting to keep me awake at night.
Any suggestions?
Thanks
Ann Hayes
Hi Ann,
For painful metacarpals I suggest you see a hand specialist… 😉
On a serious note, (and assuming you meant metatarsals), I suggest you consult a specialist who can fully assess you in person. Internet/online diagnosis is not advisable. Let me know where you are based and I will recommend someone local to you if I can.
All the best
Ian,
I have extreme pain in the ball of my feet, and find diffuculty walking. I have bunions on both feet, and have inserts. I was told that my metatarsil arches fell, causing flatness of the bottom of the ball of the foot. I would like to think that there may be something that can be done. Are you a podiatrist? Just wondering. I came online to see if there was some kind of cure, and came across your sight..leaving me discouraged at present.
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC537393/ I found some info at this site on repairing the metatarsils
Hi Carol,
The info you linked to above is 72 years old – so it’s fair to say our understanding may have improved slightly since then…
Your problem is that you ‘came online to see if there was some kind of cure’. I’m afraid that is one thing that the internet can’t do. What you need to do is see a professional who can discuss a management plan with you after diagnosing your pathology. At the moment it does not even sound like you have been given a diagnosis (‘fallen metatarsal arches’ is NOT a diagnosis).
I wish you the best of luck.
Ian.
Hi Ian,
I am a patient of the VA that has difficultly in walking. I am 68 years old. I had a stroke when I was about 47. It was a bleed that left a clot near the stem of my brain. At the time I was not a patient of the VA. I went to Albany Med. About six years ago I contracted Lyme’s disease and things started to fall apart. I had a Basel Cell Carcinoma on my chest removed.
About 5 years ago I started haveing a problem with my balance and coordination, they seemed to blame it on my drinking problem (alcohol). I went through the VA’s detox and rehab programs the last drink I had was 11/17/2008. Things got worse instead of better. I have been examined by several
phyciatrists,neurologists and a arterial surgeon. I have had
several cat-scans and MRI’s and my latest scan was last month. In December of last year I lost sight in the upper half
of my left eye. They said it was caused by a stroke in my eye. My neurologist ordered a special cat-scan with dye of my carroted arteries. What he claims is that the clot from 30 years ago had moved and was interferring with my balance and coordination. That does not explain why it feels like a rock is where my metitarsil arch used to be. Please advise me what i should do next.
Thanks, John
Hi,
I have found this quite interesting as I have had severe pains in the balls of my feet for the past 6 years and have had all kinds of treatment for Metatarsalgia – physio, injection therapy and a surgical ligament release (for Morton’s Neuroma). I have never worn high heels or narrow-toed shoes, I am at my most comfortable in bare feet or spongy flat flip flops.
I do have Morton’s Toe, my second metatarsal is longer than my first and when walking my second and third metatarsal heads hit the ground first (and have the pebble feeling when I first get out of bed in the mornings causing me to hobble around the room for a while until it adjusts itself).
I also have a clicking in the third and fourth metatarsal heads when wearing shoes and after a while of this clicking the burning pains start (usually when I am doing sports or running) and I’m limping at the end of my session until I take my shoes off.
A recent orthopaedic doctor complimented my skeleton structure and the fact that I do have nice feet with long straight toes. He diagnosed hypermobility of the metatarsal heads and flat fore feet; he prescribed a very expensive custom insole made with memory foam with a metatarsal pad in the middle to provide support to the second, third and fourth metatarsals and arch support.
These insoles kill my feet! My arches feels like there are hot knives being stabbed into them and the pad just ensures that the second and third metatarsal heads are still coming into the weight bearing first so cause me even more burning pain and more quickly.
I went out and bought a sports silicon insole with metatarsal support and taped a small 4mm thick pad (cut up foam insole) to the first metatarsal head of each foot. Then I played the first pain-free golf in 5 years able to easily walk the course in comfort. I’m playing tennis later in the week so i will have a better idea of how effective this small adjustment is.
Thank you everyone for your interesting posts. Sarah, I would like to know the brand of the metatarsal support you stuck in your shoes? Can you please share that with us? Thanks in advance.
Hi Ian,
I’ve had pain under my 2nd metatarsal on and off for 3 or 4 months – an overuse injury I believe, having done a lot of skipping (light jumping on the balls of my feet) for the last 3 years. Poor technique took its toll.
I’m trying conservative methods (rest, ice, elevation…) but the symptoms persist. When the problem started I made the mistake of exercising too soon after the symptoms subsided, and it returned.
My question is about choosing foot supports. I don’t understand how metatarsal pads can help – surely this would INCREASE pressure on the metatarsals, rather than relieve pressure? There seems to be two opposing approaches: put a “metatarsal pad” under the metatarsal area, versus padding other areas (eg. longitudinal arch) to reduce pressure under the metatarsal area.
Can you enlighten me on which approach makes most sense?
Many thanks.
Hi Andre,
Foot orthoses/inserts/padding can really only work by changing the magnitudes and locations of forces at the foot-shoe interface. What approach is best will depend on what your in-shoe intervention is actually trying to achieve.
The decision on whether foot orthoses are an appropriate part of any patients management plan, (and if so what design features may be most beneficial) will largely depend upon what the actual problem is – i.e. the diagnosis.
The anatomy in the region of the 2nd metatarsalphalangeal joint is vast. Symptoms here can be caused by a range of different pathologies; joint capsulitis/synovitis, plantar plate tears, bony stress reactions, flexor tendinopathies (to name just a few). Treatment of these injuries will vary, and as such the only online advice I would give you would be to identify what you are dealing with, and then allow that to dictate the most approriate management plan.
Hi Ian,
Thanks so much for your very helpful and clear response.
Do I risk adding long-term damage if I wait several more weeks to reach the correct diagnosis via the NHS (waiting on visits to GPs, waiting on x-ray results, getting referrals etc.).
Should I see a podiatrist privately as soon as possible to get a quicker diagnosis?
Andre
Andre,
If you are wearing sensible shoes, and have modified your activity sensibly then I very much doubt you risk any long term damage by waiting for the NHS. (Just potential frustration!)
As I’m sure you know, in the UK the main benefit of seeing someone privately is how quickly you are seen – if this high on your priority list then it may be something you wish to consider. You could see a Sports Physician, a Podiatrist, or even a Physiotherapist who specialises in the lower limb/foot. If this is something you are keen to do then let me know where you are based and I will make some recommendations if I can.
Ian
Hi again Ian,
The problem I’ve had on and off for 4-5 months now has been diagnosed by a sports podiatrist as capsulitis. I’ve stopped exercising for a couple of months and am trying conservative methods and orthotics, and I can walk without a limp now, but the problem lingers in the background.
My question is: does it become trickier to get rid of the longer it remains chronic? ie. if I opt for a cortisone shot to reduce inflammation should I do it sooner rather than later? Secondly, in your experience how often do you see a full recovery from capsulitis in 40-something sporty men with a longer 2nd toe? I hope to resume an exercise routine including running/skipping one day, but despite all my research so far I’m still unsure as to how optimistic I can be. I’m willing to do whatever it takes.
Many thanks.
Hi again Andre,
Glad to hear you have a diagnosis, and things sound as if they are progressing in the right direction for you finally.
Even with all the right things in situ (rest/activity modification, foot orthoses etc) lesser metatarsal capsulitis can take some time to fully resolve. That said, full resolution and subsequent return to sport is more often than not completely achievable, even in 40-somethings 😉
Personally, I refer a lot of these cases on for ultrasound guided injections fairly early on (concurrent to the orthoses I have issued). Have you had a chat to your Podiatrist about this as an option already?
If you want to reply privately please feel free to do so – you have my email address.
All the best.
Ian,
I went to a local podiatrist who made inserts for my feet in 2002. For the last several years I noticed that I was developing hammer toes in both feet. At various times, I had pain in the 1st & 2nd metatarsal heads on my left foot. The pain was increasing, so I recently went to see a local chiropractor who had helped me in the past. He said that I had fallen transverse arches. He did some adjustments on my feet & provided me with some inserts. My feet have never felt better and looked better. I don’t know what diagnosis or language he should or should not be using but I’m grateful.
On another note, when I told the podiatrist that my left leg was shorter than my right, he said that wasn’t the case. Medical doctors, in general, don’t listen, so I didn’t argue, however, I had had my tibias, fibulas, & femurs measured on an x-ray. Further, I know that all of my pants are not longer in the left leg.
Sylvia