8 Signs That Red, Bloodshot Eyes Need Medical Attention
Key takeaways:
There are certain signs that suggest a red eye needs medical attention.
Most serious causes of red eyes are rare, but they can cause long-term problems if left untreated.
Changes in your vision, severe pain, or symptoms that keep getting worse are reasons to see a healthcare professional right away.
Table of contents
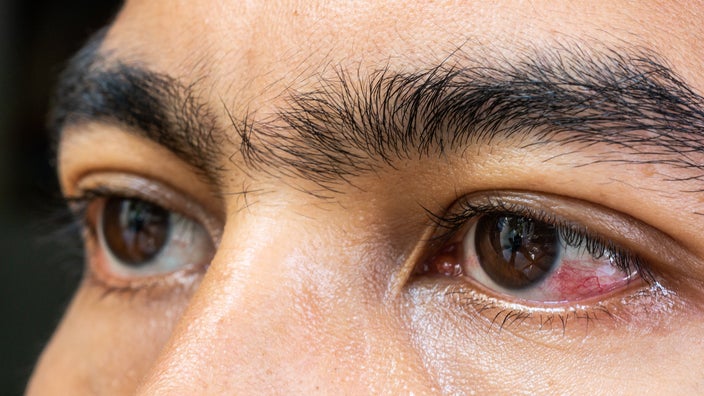
A red eye might look scary and cause discomfort. But the good news is that most episodes of red eyes are from common, less serious causes like allergies, viral infections, or dry eyes. And there are treatments to help these eye issues.
Sometimes, though, red eyes can be a sign of something more serious. Keep reading to find out when you should get medical attention for red or bloodshot eyes.
When should you get medical care for red eyes?
It can be difficult to know how much to worry about red eyes. If you experience any of the following eight signs or symptoms, it’s time to visit the doctor’s office.
1. Your vision changes or worsens
If you’re having trouble seeing, that’s a sign you need a medical evaluation. Trouble seeing can include:
Blurry or double vision
Dark spots in your vision
Flashing or twinkling lights in your vision
Your vision is worse despite using your eyeglasses or contacts.
You can’t see at all from one or both eyes.
2. You can’t open your eyes
You should get medical attention right away if you can’t open your eyes because:
They hurt too much.
They’re too sensitive to light.
The lids are swollen shut.
They seem paralyzed.
That said, if you have a mild infection or allergies, your eyes might be stuck shut with a dried crust. If so, a warm, moist cloth will dissolve the crust and allow you to open your eyes.
3. Your eyes hurt — badly
When you have dry eyes or another common eye problem, your eyes can feel gritty. But eye pain that stops you in your tracks is another story. If it hurts to move your eyes, or if you have severe pain with light sensitivity, headache, nausea, or vomiting — you should have a medical professional take a look.
4. You got something in your eye
Sometimes an eye injury is obvious, but other times it can sneak up on you. Chemical splashes and splinters tend to cause damage over time. Your eye might seem fine for several hours, then it may start to turn red later on.
If you know you got something in your eye, rinse it with lots of water as soon as possible. If your eye still doesn’t seem right, that’s worth a closer examination.
5. You wear contacts, and removing them didn’t help
People who wear contacts are at high risk for serious eye infections. If your eye redness isn't any better after you take your contacts out — and especially if the redness seems worse — you’ll want to get a medical evaluation right away.
6. You recently had surgery on your eye
Right after eye surgery, your eye will be red and swollen for a while — but it will get better over time. Eye redness or pain that gets worse instead of better after surgery could be cause for concern. If you’re not sure, talk with your surgeon right away.
7. You have other signs of a serious infection
Most cases of mild conjunctivitis don’t need medical treatment, but stronger infections do. If you have discharge from your eye, especially if it looks like thick pus, that could be one sign of a strong infection. Or if you have swelling and redness of the skin around your eye, you likely need professional care for an eye infection.
8. The redness is getting worse, not better
Sometimes the pattern of your symptoms can tell you a lot about the problem. For example, a healing corneal abrasion (scratch on the eye) will get better over time. A corneal ulcer, on the other hand, will get worse. In general, symptoms that don’t improve over time need to be checked out.
What are the more serious causes of red eyes?
The symptoms listed above could point to serious medical problems. Serious medical problems of the eye can be infectious, inflammatory, traumatic, or a sign of a more general medical condition. Let’s review some of the more serious causes of red eyes.
Infectious causes of red eyes
Infections are caused by germs that get into the eye or eyelid. Mild viral eye infections don’t usually need medical treatment, but most other types do.
Bacterial conjunctivitis
Conjunctivitis, or “pink eye,” is inflammation of the conjunctiva, which is the thin, clear lining that covers the white of the eye and inside the eyelid. When bacteria causes conjunctivitis, it leads to pus or thick, yellow eye drainage.
Chemical conjunctivitis
Chemical conjunctivitis is caused by liquids, powders, smoke, or fumes that enter the eye. It requires medical treatment.
Severe viral conjunctivitis
Viral conjunctivitis usually causes thin, mucousy eye drainage. It often comes with cold-like symptoms, such as a runny nose, congestion, and fever. Viral conjunctivitis is usually mild, but sometimes it can be severe. When this happens, the eye looks very red, feels irritated, and is quite sensitive to light. It’s difficult to tell the difference between severe viral and other types of conjunctivitis. If you’re not sure, it’s best to get a medical evaluation.
Orbital and periorbital cellulitis
Orbital and periorbital cellulitis are infections of the eyelid and the area around the eyeball. They can cause redness, swelling, pain, and fevers. They’re usually caused by bacteria.
Eyelid stye
Inflammation and infection of the glands along the edge of the eyelid can cause styes. A stye looks like a red bump or pimple right where the eyelashes grow. Styes can often be treated at home, but medical care is helpful when styes don’t go away quickly, or if they come back frequently.
Corneal ulcer
Corneal ulcers are open sores on the surface of the cornea. They occur when germs enter the eye and they can cause permanent damage. Corneal ulcers are often the result of eye trauma, contact lens overuse, or a corneal abrasion.
Endophthalmitis
Endophthalmitis is an infection inside the eyeball. It’s a medical emergency. Endophthalmitis can start after an eye injury, eye surgery, or an injection into the eye — or it can spread from an infection elsewhere in the body. Symptoms are usually severe pain and vision loss.
Inflammatory causes of red eyes
There are times when inflammation affects the eyes. This can cause symptoms similar to an infection, but antibiotics and other germ-fighting medications aren’t helpful. Occasionally these are signs of an underlying medical condition.
Eyelid inflammation (blepharitis)
When the eyelid edge becomes inflamed, it can affect the eyes and cause redness. Dirt, oil, makeup, and other debris around the eyelashes can contribute to blepharitis. Sometimes blepharitis is related to skin conditions like rosacea.
Scleritis or episcleritis
Episcleritis is inflammation of the sclera (white part of the eye). Scleritis is similar but more severe. These conditions can affect either one eye or both eyes at once, and severe cases can be very painful. Scleritis and episcleritis can sometimes be linked to autoimmune conditions like lupus or rheumatoid arthritis.
Uveitis
Uveitis is inflammation and swelling of the uvea, or middle layer of the eye. When the back of the eye or retina is involved, uveitis might cause flashes of light or black spots in your vision. Like episcleritis or scleritis, uveitis is sometimes linked to autoimmune disorders, but it can have other causes, too.
Keratitis
Keratitis is inflammation and swelling of the cornea, the clear dome that covers the colored part of your eye. Sometimes keratitis is triggered by infections from bacteria, viruses (like herpes simplex virus), or fungi. But it can also occur after eye injury or overexposure to ultraviolet light.
Traumatic causes of red eyes
Although trauma to the eye is often obvious, it doesn’t have to be. Sometimes very small eye injuries can lead to bigger problems.
Corneal abrasions
Corneal abrasions are cuts or scrapes on your cornea. These are often caused by:
Fingernails
Debris, like sand, wood, and tree branches
Fragments of metal (especially if you work with it)
Hair and makeup brushes
Foreign bodies
Foreign bodies are particles in the eye. They might stay on the surface of the eye and under the eyelid, or they can move deeper and can cause permanent damage.
Trichiasis
Sometimes eyelashes grow in a way that points them toward the eyeball, instead of away from it. When this happens, the lashes might scratch the eye surface during blinking. This condition results in corneal abrasions and needs treatment.
Photokeratitis
When the eyes are damaged due to exposure to UV light, the result is photokeratitis. This is sometimes thought of as a sunburn to the eyes, and it can be quite painful.
Other general causes of red eyes
A variety of other general and eye-specific conditions can cause your eyes to look red.
Subconjunctival hematoma
A bright red splotch on the white part of the eye is often a subconjunctival hematoma or hemorrhage. This happens when a blood vessel on the surface of the eye breaks and bleeds underneath the conjunctival membrane. Straining, coughing, or vomiting can lead to subconjunctival hematomas. Usually they don’t need treatment, but sometimes they can be one sign of low platelets or a bleeding or clotting disorder.
Acute angle-closure glaucoma
Acute angle-closure glaucoma occurs when eye pressure builds quickly, damaging the optic nerve at the back of the eye. This can cause vision loss, severe headaches, and nausea or vomiting. It’s a medical emergency, so get help right away if you have these symptoms.
Ocular rosacea
Rosacea is a common skin condition that causes redness and irritation on the face. When it happens near the eyes, it can contribute to blepharitis. It’s still not clear what the underlying causes of rosacea are, but it seems likely that inflammation and/or infection play a role.
Retinoblastoma
This rare eye cancer doesn’t usually cause red eyes — although it can. It runs in families and is most common in children. If you’re worried about retinoblastoma, it’s worth discussing your concerns with a medical professional.
WHAT TO READ NEXT
How does a doctor diagnose serious causes of red eye?
First, a healthcare professional will ask you questions about your symptoms. Then they’ll examine your eyes and check your vision.
Testing with special equipment is often helpful. This could include:
Ophthalmoscope: Ophthalmoscope is a magnifying lens and flashlight used to look inside the eye (often through a dilated pupil).
Wood’s lamp: Wood’s lamp is an ultraviolet light that can show corneal abrasions, ulcers, and keratitis.
Slit lamp: This is a magnifier with a strong beam of light focused into a vertical line. A slit lamp reveals details on the surface of the eye.
Tonometer: A tonometer measures the pressure inside of your eye to check for glaucoma.
Ultrasound: An ultrasound checks structures inside of the eye.
They might also order lab tests to look for infection or autoimmune disease. In some cases, you might get a referral to an eye specialist for more evaluation.
The bottom line
Red eyes are very common and can be caused by allergies, viral infections, or dry eyes. But sometimes they’re the result of more serious conditions that need medical attention. In general, reasons to get professional help include severe pain, changes in your vision, or symptoms that keep getting worse. An eye exam by a medical professional is critical for getting the right diagnosis and treatment.
References
Abu-Hassan, D. W., et al. (2014). The trabecular meshwork: A basic review of form and function. Journal of Ocular Biology.
Al Aboud, D. M., et al. (2023). Wood's light. StatPearls.
American Academy of Ophthalmology. (2016). Cornea.
American Academy of Ophthalmology. (2016). Sclera.
Austin, A., et al. (2017). Update on the management of infectious keratitis. Ophthalmology.
Bader, J., et al. (2021). Tonometry. StatPearls.
Boyd, K. (2023). What is a subconjunctival hemorrhage? American Academy of Ophthalmology.
Boyd, K. (2024). What is retinoblastoma? American Academy of Ophthalmology.
Boyd, K. (2024). What is trichiasis? American Academy of Ophthalmology.
Centers for Disease Control and Prevention. (2021). Conjunctivitis (pink eye).
Grzybowski, A., et al. (2019). Postoperative endophthalmitis is the most severe complication of cataract surgery. ResearchGate.
Gupta, Y., et al. (2023). Post injection endophthalmitis (PIE). EyeWiki.
Heiting, G. (2022). Iris/uvea of the eye. All About Vision.
Johnson, L. (2019). Ocular ultrasound. Core EM.
Koviak, K. (2015). Perforated corneal ulcer. Kellogg Eye Center.
National Eye Institute. (2021). Get a dilated eye exam.
National Health Service. (2020). Uveitis: Causes.
Patel, S. J., et al. (2002). Ocular manifestations of autoimmune disease. American Family Physician.
Porter, D. (2018). What is a slit lamp? American Academy of Ophthalmology.
Porter, D. (2021). What is photokeratitis – including snow blindness? American Academy of Ophthalmology.
Roat, M. I. (2022). Herpes simplex keratitis. Merck Manual: Consumer Version.
Roat, M. I. (2022). Herpes simplex keratitis. Merck Manual: Professional Version.
Stanford Medicine 25. (n.d). Fundoscopic / ophthalmoscopic exam.
Vislisel, J. (2015). Corneal abrasion. University of Iowa Healthcare.
Zagaria, M. A. E. (2016). Postoperative endophthalmitis after cataract surgery. U.S Pharmacist.