Decoding an Abnormal ECG: Premature Ventricular Contractions (PVCs)
Key takeaways:
Premature ventricular contractions (PVCs) are a common finding on ECGs (electrocardiograms). They’re an extra heartbeat that is out of sync with the normal heart rhythm.
PVCs can occur in a healthy heart, and most of the time they’re not dangerous. But in certain cases, they can be a sign of a heart or medical condition.
Most people do not need treatment for PVCs. But your provider may do more testing to look for a cause of your PVCs.
If you recently had an ECG (electrocardiogram), you may have been told that yours is “abnormal.” Naturally, you might worry that something serious is going on in your heart. But this is more common than you think. Almost everyone who gets their heart monitored for more than a few hours has an occasional weird heartbeat known as a “premature ventricular contraction” (PVC).
Most of the time, PVCs on an ECG are not a sign of a bigger problem with your heart. But, in some cases, they can be a clue that something else is going on. We’ll explain exactly what a PVC is and what you need to know if you have this abnormality on your ECG.
What is happening in the heart during a premature ventricular contraction (PVC)?
A PVC occurs when the lower chambers of the heart try to sneak in an extra heartbeat. This extra beat is out of rhythm with the normal heartbeat. It then causes the heart to briefly “reset” its rhythm to get all of the heart chambers back in line.
It may help to think of the heart like a marching band. The field commander is like the pacemaker of the heart — it sets the pace and tone for the entire band. But, from time to time, a band member steps out of line. This can mess up the rhythm of the whole group. The field commander then needs to get the group back in line.
A PVC is like a little band member stepping out of line. It causes an early beat that’s not in sync with the rest of the heartbeats. It’s usually followed by a pause (a reset), then a really strong heartbeat. There are a few theories about what actually causes a PVC, but most of the time there’s no obvious cause.
What do PVCs look like?
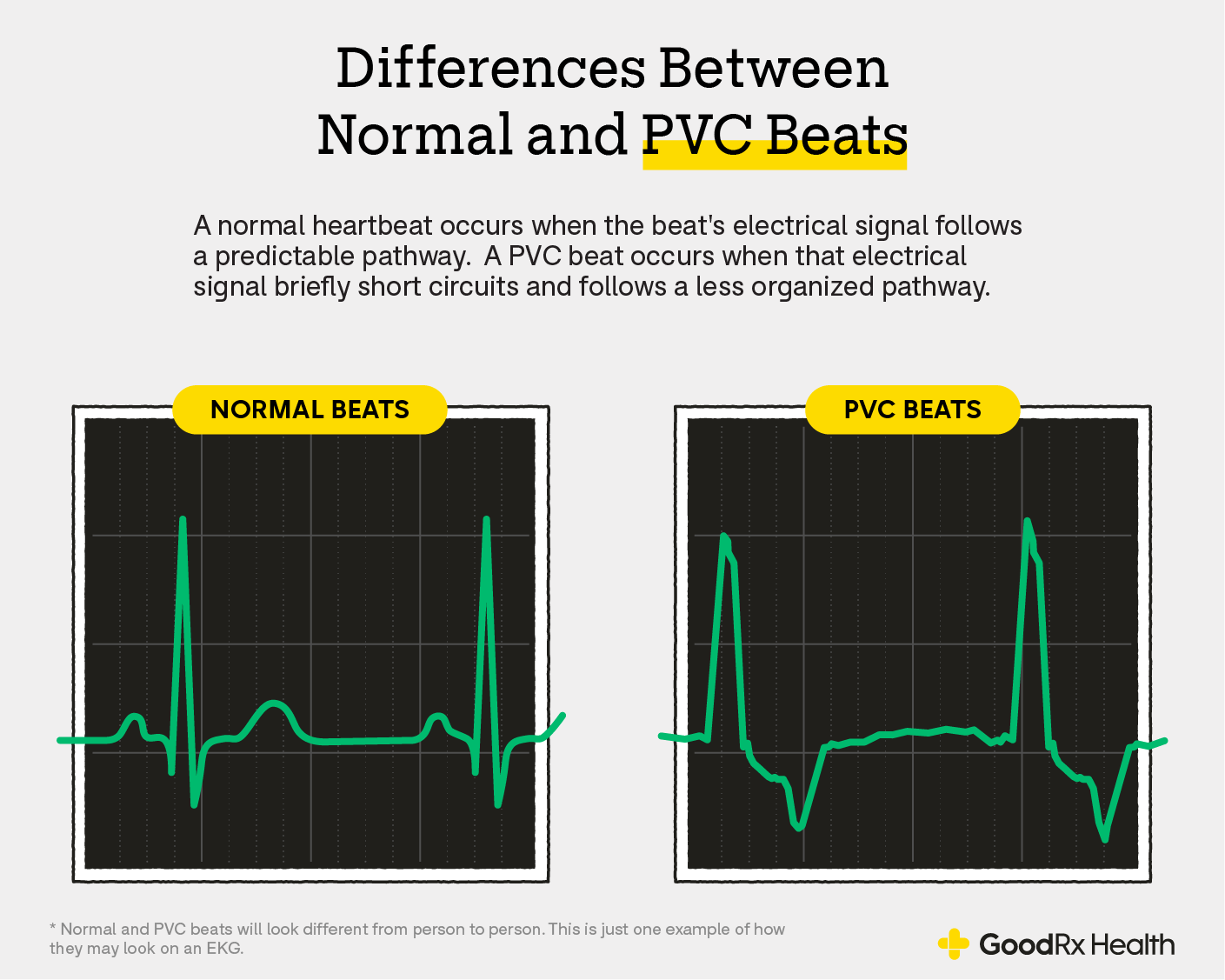
If you have a PVC, it will cause your ECG to look slightly abnormal. But it will only look abnormal at the part where the extra beat occurs and right after, when the heart is resetting.
ECGs are essentially 10-second snapshots of your heart rhythm. Each heartbeat translates to a wave on the ECG paper.
A regular heartbeat is called a “sinus beat.” It looks narrow and concise. A PVC usually appears wider, taller, and a little more erratic. In other words, a sinus beat is tight and well packaged. And a PVC beat is loose and a little messy. It’s also usually followed by a briefly longer pause before the normal sinus beat resumes.
What causes PVCs?
Usually there isn’t any obvious cause of a PVC — and it’s probably a bit different for every heart. But researchers have figured out some things that are associated with a higher rate of PVCs. These include:
Male anatomy
Taller height
Black race
Elevated BMI
Smoking
Less regular physical activity
Higher resting heart rate
Hypertension
Coronary artery disease or prior heart attack
Heart arrhythmias (abnormal heart rhythm)
Electrolyte imbalances, like low levels of magnesium or potassium
Heart conditions, like heart failure
How common are PVCs?
Many people have PVCs and don’t even know it. In healthy people, PVCs are seen about 1% of the time with routine ECGs.
But PVCs are more likely to be detected when someone is monitored for longer. When monitored for 24 hours, more than 50% of healthy people will have a PVC! One study even found at least one PVC in 69% of participants who were monitored at home for 24 hours.
Even though occasional PVCs are common, it’s very unlikely to see PVCs in more than 20% of heartbeats.
How do you diagnose PVCs?
Routine ECGs can easily pick up PVCs. And people get ECGs for a wide range of reasons. So PVCs are often an incidental finding. They may also be discovered when someone is hooked up to a heart rate monitor — like during surgery or a hospital stay.
PVCs can also be found on a workup for heart disease. PVCs can cause palpitations in some people, so they may be detected when a provider is looking for signs of a heart arrhythmia.
PVCs can also be associated with heart disease. So they may be picked up during a workup for symptoms like:
Dizziness of feeling faint
Shortness of breath
Chest discomfort
General weakness or fatigue
What testing may be needed after a diagnosis of PVCs?
Though PVCs are common and normal in healthy individuals, a high frequency of PVCs is a different story. When over 20% of someone’s heartbeats are PVCs, this is more likely to be associated with a heart condition — like heart failure or coronary artery disease.
So even though your PVCs may not be dangerous, your provider may want to do some testing to look for an underlying cause.
Many times, the next test is an echocardiogram. This is an ultrasound of the heart. It takes a close look at the size and shape of the heart and how well it is pumping. It can diagnose heart disease, like heart failure.
Your provider may also recommend additional testing. This will depend on your other medical conditions, family history, and the frequency of your PVCs. Further testing may include:
Blood tests to look for electrolyte abnormalities
A stress test of the heart
A cardiac MRI to take a closer look at heart muscle and heart structure
Electrophysiologic testing — when a cardiologist looks at the electric circuitry of the heart
Do you need treatment if you’re diagnosed with PVCs?
In most people, a PVC is a routine finding that doesn’t need treatment. This is especially true if your heart is healthy and your PVCs don’t occur frequently.
You and your provider may discuss other medical conditions or lifestyle factors that could be contributing — like smoking or high blood pressure. In that case, they may recommend treatment or lifestyle changes.
But you may need treatment if your PVCs are associated with an underlying heart condition. If your heart function is abnormal, PVCs can put extra stress on the heart. And this can lead to heart failure. So your provider may recommend a medication like a beta blocker to reduce the frequency of your PVCs.
And, of course, if you have an underlying heart condition, it will be important to treat that condition.
The bottom line
If you have recently been diagnosed with PVCs on your ECG, don’t worry. Almost everyone has PVCs! And, most of the time, they’re not a sign of heart disease. But it’s still important to follow up with your provider to find out if you need more testing to rule out other heart conditions. And if you’re experiencing any new symptoms — like chest pain or shortness of breath — don’t wait. See your provider right away.
References
Agarwal, V., et al. (2012). Relation between ventricular premature complexes and incident heart failure. The American Journal of Cardiology.
Dong, Y., et al. (2022). Prevalence and heart rate variability characteristics of premature ventricular contractions detected by 24-hour Holter among outpatients with palpitations in China: a cross-sectional study. The BMJ.
Hiss, R. G., et al. (2016). Electrocardiographic findings in 122,043 individuals. Circulation.
Kostis, J. B., et al. (1981). Premature ventricular complexes in the absence of identifiable heart disease. Circulation.
Marcus, G. M., et al. (2020). Evaluation and management of premature ventricular complexes. Circulation.
Simpson, R. J., et al. (2002). Prevalence of premature ventricular contractions in a population of african american and white men and women: The Atherosclerosis Risk in Communities (ARIC) study. American Heart Journal.
Sobotka, P. A., et al. (1981). Arrhythmias documented by 24-hour continuous ambulatory electrocardiographic monitoring in young women without apparent heart disease. American Heart Journal.
Yang, J., et al. (2014). Characteristics of unselected high-burden premature ventricular contraction patients. Pacing and Clinical Electrophysiology.