Anatomy Review
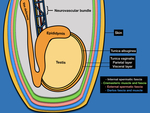
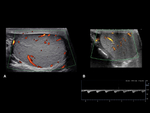
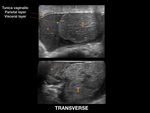
The scrotal sac is divided at midline by a septum, each half containing a testis and associated structures [2]. The scrotal sac has several layers that cannot be distinguished using US Fig. 1. The tunica vaginalis is composed of two layers: the parietal layer lining the scrotal wall and the visceral layer lining the testicle and epididymis [1,2,7]. The space between the layers of the tunica vaginalis creates a potential space for fluid accumulation. The visceral layer of the tunica vaginalis adheres to the tunica albuginea, which further creates septa invaginating into the testicle and creating different lobules.
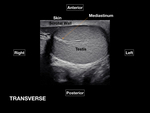
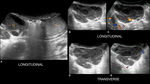
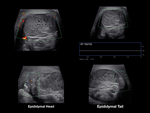
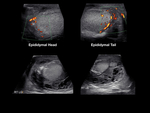
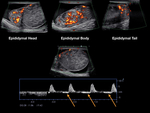
Inside each lobule, seminiferous tubules merge to form the rete testis, structure located at the mediastinum of the testicle. The rete testis drains into the efferent tubules that converge to form the epididymis. The epididymis is divided into head, body, and tail. The head of the epididymis is located on the superior aspect of the testis, while the body and tail extend to the inferior aspect of the testis [7]. Fig. 2 Fig. 3
Stepwise Sonographic Evaluation of the Scrotum
-
How to position the patient?
-
The patient should be positioned supine on the examination bed, with a rolled towel placed under the scrotum for testicular support. The penis should be displaced upward to provide better visualization [6]. Drapes are placed on top of the penis and around the thighs, with only the scrotum uncovered for the examination.
-
Which transducer to use?
-
A linear high frequency transducer (8-15MHz) [6].
-
What areas need to be evaluated?
-
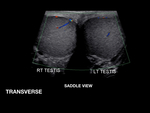
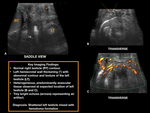
Obtain a saddle view Fig. 4, which is a midline transverse view with both testicles.
-
Start unilateral evaluation with non-affected hemiscrotum, then proceed with affected hemiscrotum.
-
Each hemiscrotum is scanned longitudinally and transversely.
-
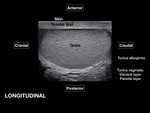
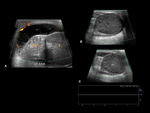
The anteroposterior (AP) and craniocaudal measurements of the testicle are taken in the longitudinal view Fig. 5.
-
The transverse diameter of the testicle is measured at mid testicle Fig. 5.
-
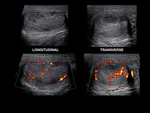
Evaluate echotexture, skin thickness, and color Doppler flow pattern [6] Fig. 6.
-
Evaluate the head, body, and tail of the epididymis.
See Fig. 7 for details regarding sonographic appearance of the scrotum.
Sonographic Findings of Acute and Post-Surgical Scrotal Emergencies
Scrotal Trauma
Scrotal trauma accounts for less than 1% of all trauma-related injuries with a peak occurrence in the age range of 10-30 years [7] Fig. 8. US is useful in the triage of patients for medical or surgical management because it reliably depicts tunica albuginea rupture, intra- and extratesticular hematomas, and testicular contusions [4].
Scrotal Wall Hematoma
Scrotal wall thickening is commonly associated with blunt scrotal trauma. Hematomas are also a common finding and may appear as focal thickening of the scrotal wall or as fluid collections within the scrotal wall Fig. 9. Hematomas appear echogenic on US when acute and evolve with age [9].
Hematocele
Patients with scrotal trauma may have scrotal discoloration or a tender, firm scrotal mass that fails to transilluminate. This could indicate a hematocele, which occurs when the tunica vaginalis fills with blood [6].
Hematoceles are complex collections that separate the visceral and parietal layers of the tunica vaginalis Fig. 10. Like hematomas, they are acutely echogenic and become more complex and more hypoechoic with age. Subacute and chronic hematoceles may contain fluid-fluid levels or low-level internal echoes [7].
Tunica Albuginea Rupture
Testicular rupture is defined as a tear of the tunica albuginea with protrusion of the seminiferous tubules Fig. 11. The normal tunica albuginea in US appears as a thin echogenic line surrounding the testicular parenchyma Fig. 2. When testicular rupture is present, the hyperechoic tunica albuginea is interrupted, and there is an extrusion of testicular tissue into the scrotum. Heterogeneous parenchymal echotexture and irregular margins are typical characteristics of testicular rupture [5]. Rupture of the testis results in a loss of vascularity to a portion or the entirety of the testis on color Doppler, depending on the grade of injury Fig. 12.
Intratesticular Hematoma
Intratesticular hematomas are usually focal, well defined and may be single or multiple Fig. 13. On ultrasound examination, hyperacute and acute hematomas are sometimes difficult to identify, as they may appear isoechoic to the surrounding testicular parenchyma or may have diffusely heterogeneous echotexture. Suspected acute hematomas are re-examined within 12-24 hours after initial US evaluation to allow observation of any changes in their echogenicity [4].
Hematomas demonstrate an absence of internal vascularity, but when infected, an increase in peripheral vascularity may be noted [4] Fig. 14. Follow-up US of conservatively treated intratesticular hematomas is essential because of the high incidence rate (as much as 40%) of infection and necrosis, which may require an orchiectomy [4].
Testicular Torsion
Testicular torsion is the result of twisting of the spermatic cord causing first venous congestion, then a decrease in the arterial flow that can lead to ischemia. There are two types of testicular torsion: extravaginal torsion that occurs exclusively on the neonatal period and intravaginal torsion that most commonly occurs between 12-18 years. Patients present with acute unilateral scrotal pain and can have associated systemic symptoms like nausea and vomiting [6].
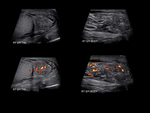
Intravaginal torsion is caused by the twisting of the spermatic cord inside the tunica vaginalis Fig. 15. US findings of the affected testis include diminished or absent flow on color Doppler Fig. 16, testicular enlargement, twist of the spermatic cord known as “whirlpool sign” [3], torsion knot complex Fig. 17, reactive hydrocele and skin thickening. During the first 4-6 hours after the onset of symptoms, the testicle has a decreased echogenicity. As time progresses, there is a change to heterogeneous echotexture caused by areas of necrosis and areas of hemorrhage [1].
Torsed Appendage
Testicular torsion should be differentiated from a torsed testicular or epididymal appendage Fig. 18. US findings include a heterogeneous area near the superior aspect of the testicle Fig. 18, a reactive hydrocele or skin thickening [1, 6].
Infectious Process
Epididymitis and Epididymo-orchitis are the result of an infectious process affecting the epididymis and eventually spreading to the testis Fig. 19. US findings include an enlarged heterogeneous epididymis with increased flow on color doppler Fig. 20, a reactive hydrocele, and scrotal skin thickening [1]. Severe cases of epididymitis can lead to complex hydrocele formation Fig. 21, intratesticular abscess formation Fig. 14, and vascular insult of the testicle Fig. 22.