Abstract
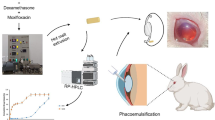
Hydroxyethyl chitosan (HECTS) is a critical derivative of chitosan that has been widely used as biomedical materials due to great water-solubility and excellent biocompatibility. Here, photosensitive hydroxyethyl chitosan was synthesized by introducing azide group on NH2 of HECTS (HECTS-AZ), afterwards FTIR and 1H NMR spectra were detected to confirm the formation of HECTS-AZ. The solution of HECTS-AZ can achieve a sol–gel transition through UV irradiation for 30 s. The evaluation of biocompability and biodegradability in vivo was conducted in rats, visual and pathological examinations exhibited the HECTS-AZ has excellent biocompability and degradation time of the hydrogel is more than 14 weeks. Furthermore, HECTS-AZ hydrogel as an ocular drug delivery system loading heparin was prepared to implant under sclera of rabbit after glaucoma filtration surgery (GFS). The experimental results demonstrated the heparin loaded hydrogel can effectively maintain filtration bleb and lowing intraocular pressure (IOP) after GFS for prolonged time. Besides, obvious inflammatory reactions and side effects have not been observed in ocular during the experimental period. In conclusion, the HECTS-AZ hydrogel is a potential drug delivery device for the treatment of glaucoma and other ocular diseases.
Graphical abstract







Similar content being viewed by others
References
Quigley HA, Broman AT. The number of people with glaucoma worldwide in 2010 and 2020. Br J Ophthalmol. 2006;90:262–7.
Cohen LP, Pasquale LR. Clinical characteristics and current treatment of glaucoma. Cold Spring Harb Perspect Med. 2014;4(6):256–60.
Kim M, Lee C, Payne R, et al. Angiogenesis in glaucoma filtration surgery and neovascular glaucoma-a review. Surv Ophthalmol. 2015;60(6):524–35.
Robin AL, Ramakrishnan R, Krishnadas R, et al. A long-term dose-response study of mitomycin in glaucoma filtration surgery. Arch Ophthalmol. 1997;115(8):969–74.
Skuta GL, Beeson CC, Higginbotham EJ, et al. Intraoperative mitomycin versus postoperative 5-fluorouracil in high-risk glaucoma filtering surgery. Ophthalmology. 1992;99(3):438–44.
Fan SQ, Qin LY, Cai JL, et al. Effect of heparin on production of basic fibroblast growth factor and transforming growth factor-beta1 by human normal skin and hyperplastic scar fibroblasts. J Burn Care Res. 2007;28(5):734–41.
Xi L, Wang T, Zhao F, Zheng Q, Li X, Luo J, et al. Evaluation of an injectable thermosensitive hydrogel as drug delivery implant for ocular glaucoma surgery. PLoS ONE. 2014;9(6):e100632.
Whittlesey KJ, Shea LD. Delivery systems for small molecule drugs, proteins, and DNA: the neuroscience/biomaterial interface. Exp Neurol. 2004;190(1):1–16.
Lai JY. Biocompatibility of chemically cross-linked gelatin hydrogels for ophthalmic use. J Mater Sci Mater Med. 2010;21(6):1899–911.
Katiyar S, Pandit J, Mondal RS, et al. In situ gelling dorzolamide loaded chitosan nanoparticles for the treatment of glaucoma. Carbohydr Polym. 2014;102(1):117–24.
Hoffman AS. Hydrogels for biomedical applications. Ann N Y Acad Sci. 2001;54(944):62–73.
Bhattarai N, Matsen FA, Zhang M. PEG-grafted chitosan as an injectable thermoreversible hydrogel. Macromol Biosci. 2005;5(2):107–11.
Aziz MA, Cabral JD, Brooks HJL, et al. In vitro, biocompatibility and cellular interactions of a chitosan/dextran-based hydrogel for postsurgical adhesion prevention. J Biomed Mater Res B Appl Biomater. 2015;103(2):332–41.
Kozicki M, Kołodziejczyk M, Szynkowska M, et al. Hydrogels made from chitosan and silver nitrate. Carbohydr Polym. 2016;140:74–87.
Ishihara M, Nakanishi K, Ono K, et al. Photocrosslinkable chitosan as a dressing for wound occlusion and accelerator in healing process. Biomaterials. 2002;23(3):833–40.
Hattori H, Amano Y, Nogami Y, et al. Hemostasis for severe hemorrhage with photocrosslinkable chitosan hydrogel and calcium alginate. Ann Biomed Eng. 2010;38(12):3724–32.
Shao K, Han B, Gao J, et al. Synthesis and characterization of a hydroxyethyl derivative of chitosan and evaluation of its biosafety. J Ocean Univ China. 2015;14(4):703–9.
Peng R, Qin G, Li X, et al. The PEG-PCL-PEG hydrogel as an implanted ophthalmic delivery system after glaucoma filtration surgery; a pilot study. Med Hypothesis Discov Innov Ophthalmol. 2014;3(1):3–8.
Liang L, Xu XD, Chen CS, et al. Evaluation of the biocompatibility of novel peptide hydrogel in rabbit eye. J Biomed Mater Res B Appl Biomater. 2010;93(2):324–32.
Zhu X, Xu D, Zhu X, et al. Evaluation of chitosan/aptamer targeting TGF-β receptor II thermo-sensitive gel for scarring in rat glaucoma filtration surgery. Invest Ophthalmol Vis Sci. 2015;56(9):5465–76.
Cho IS, Park CG, Huh BK, et al. Thermosensitive hexanoyl glycol chitosan-based ocular delivery system for glaucoma therapy. Acta Biomater. 2016;39:124–32.
Raftery R, O’Brien F, Cryan SA. Chitosan for gene delivery and orthopedic tissue, engineering applications. Molecules. 2013;18(18):5611–47.
Kunio NR, Riha GM, Watson KM, et al. Chitosan based advanced hemostatic dressing is associated with decreased blood loss in a swine uncontrolled hemorrhage model. Am J Surg. 2013;205(5):505–10.
Dalirfardouei R, Karimi G, Jamialahmadi K. Molecular mechanisms and biomedical applications of glucosamine as a potential multifunctional therapeutic agent. Life Sci. 2016;152:21–9.
Nawrotek K, Tylman M, Decherchi P, et al. Assessment of degradation and biocompatibility of electrodeposited chitosan and chitosan-carbon nanotube tubular implants. J Biomed Mater Res A. 2016;104A:2701–11.
Chen Y, Liu YF, Tan HM. Hydroxyethyl chitosan- g –poly (acrylic acid- co -sodium acrylate) superabsorbent polymers. J Appl Polym Sci. 2010;117(4):2233–40.
Heo J, Koh RH, Shim W, et al. Riboflavin-induced photo-crosslinking of collagen hydrogel and its application in meniscus tissue engineering. Drug Deliv Transl Res. 2016;6(2):148–58.
Monier M, Wei Y, Sarhan AA, et al. Synthesis and characterization of photo-crosslinkable hydrogel membranes based on modified chitosan. Polymer (Guildf). 2010;51(5):1002–9.
Ishihara M, Obara K, Ishizuka T, et al. Controlled release of fibroblast growth factors and heparin from photocrosslinked chitosan hydrogels and subsequent effect on in vivo vascularization. J Biomed Mater Res A. 2003;64(3):551–9.
Henise J, Hearn BR, Ashley GW, et al. Biodegradable tetra-PEG hydrogels as carriers for a releasable drug delivery system. Bioconjug Chem. 2015;26(2):270–8.
Del Vecchio PJ, Bizios R, Holleran LA, et al. Inhibition of human scleral fibroblast proliferation with heparin. Invest Ophthalmol Vis Sci. 1988;29(8):1272–6.
Lavik E, Kuehn MH, Kwon YH. Novel drug delivery systems for glaucoma. Eye. 2011;25(5):578–86.
Acknowledgements
This work was supported by Ocean University of China and by a grant from the Key Research & Development Program of Shandong Province (2016GSF115003). And Independent Innovation and Achievement Transformation Program of Shandong Province (2014ZZCX06203).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Rights and permissions
About this article
Cite this article
Qiao, X., Peng, X., Qiao, J. et al. Evaluation of a photocrosslinkable hydroxyethyl chitosan hydrogel as a potential drug release system for glaucoma surgery. J Mater Sci: Mater Med 28, 149 (2017). https://doi.org/10.1007/s10856-017-5954-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10856-017-5954-z